During the follicular phase of the ovarian cycle, the growth and differentiation of follicles are processes subjected to a delicate and precise balance between the levels of circulating hormones and the production of their receptors in the follicular cells. If the levels of circulating hormones and the appearance of their receptors coincide, then follicular development can continue; vice versa, if this condition is not reached, the follicles undergo degeneration and the formation of atretic bodies of the ovary.
Hormonal regulation is a fundamental control mechanism of the ovarian cycle.
There are five hormones that participate in the complex positive and negative feedback process to regulate folliculogenesis:
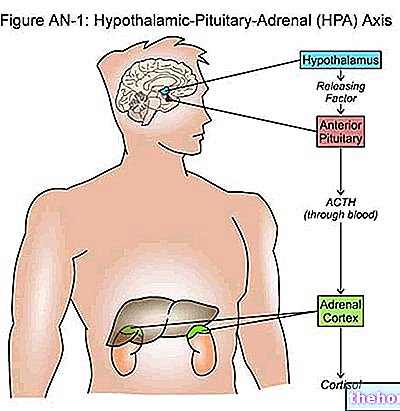
- gonadotropin-releasing hormone (GnRH) secreted by the hypothalamus
- follicle-stimulating hormone (FSH)
- luteinizing hormone (LH)
- estrogen
- progesterone
The hormones produced by the pituitary gland (FSH and LH) and the hormones produced by the ovary (estrogen and progesterone) have antagonistic effects (negative feedback control).
At the same time, to transform the continuous production of primary follicles into the periodic phenomenon of ovulation, at least two positive feedback mechanisms must intervene:
- antral phase: exponential production of estrogen;
- preovulatory phase: exponential production of FSH and LH.

Oogenesis and follicular development
Follicle-stimulating hormone (FSH) is a protein hormone that is secreted by the anterior lobe of the pituitary and acts on the gonads. FSH secretion begins to increase in the last days of the menstrual cycle, and is highest during the first week of the follicular phase. The increase in FSH levels allows the recruitment of about 10 follicles in the antral phase (Graafian follicles) for entry into the menstrual cycle. These follicles, induced to folliculogenesis, are in competition with each other for domination (only one mature egg will be released during ovulation).
The FSH hormone binds to the receptors of granulosa cells, promoting their growth and proliferation, causing an increase in the size of the follicles. Furthermore, the same hormone induces the expression of receptors for luteinizing hormone (LH) on the membrane of granulosa cells in developing follicles.
Under the influence of FSH, the enzyme estrogen synthetase and cytochrome P450 are activated, which stimulate the cells of the granulosa to the secretion of estrogen.
This increase in the level of estrogen stimulates the production of gonadotropin releasing hormone (GnRH), which induces the release of the gonadotropins FSH and LH from the anterior pituitary lobe, which exert a stimulating effect on follicle growth.
L "luteinizing hormone (LH) exerts the following actions:
- activates the synthesis of androgens by the cells of the theca (outermost layer of the granulosa cells). The secreted androgens are then brought to the level of the granulosa cells to be converted into estrogen;
- stimulates the proliferation, differentiation and secretion of theca follicular cells;
- increases the expression of LH receptors on the membrane of granulosa cells.
Increased estrogen
Two to three days before LH levels begin to rise, typically around the seventh day of the cycle, one of the recruited follicles emerges as dominant.
Estrogens perform a "negative feedback action on the hypothalamus and the anterior lobe of the pituitary": the dominant follicle secretes estrogen in large quantities, at such a level that the production of GnRH is suppressed, consequently inhibiting the secretion of LH and FSH.
This decrease in the production of the hormones LH and FSH leads to the atresia (death) of most of the non-dominant follicles.
During the early and intermediate stages of the follicular phase, estrogen promotes a variety of physiological changes throughout the body, including changes in the uterine environment characteristic of the proliferative phase.
The same hormones also promote changes that prepare the body for subsequent events in the menstrual cycle:
- during the entire follicular phase, the rise in the level of estrogen in the blood stimulates the formation of a new layer of endometrium and myometrium of the uterus;
- they induce the expression of progesterone receptors on endometrial cells, helping the endometrium to respond to increasing levels of progesterone during the late proliferative phase and throughout the luteal phase.
Pico of LH and ovulation
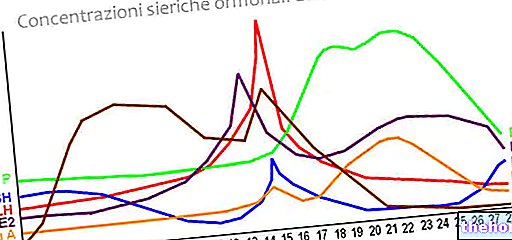
At low concentrations, estrogens inhibit gonadotropins, while at high concentrations they stimulate their release. In the late follicular phase, the production of estrogen increases exponentially, affecting the secretory activity of the hypothalamus and the anterior lobe of the pituitary, and leading to the stimulation of the secretion of luteinizing hormone (LH).
These events result in a positive feedback circuit: LH levels increase, estrogen secretion is further stimulated, therefore the release of luteinizing hormone is further promoted. LH secretion increases dramatically, resulting in an ascending phase of LH levels in the plasma (preovulatory LH surge). Under the influence of the LH surge, the endocrine activity of the thecal cells is first stimulated and then progressively shut down. At this point, the LH hormone induces these cells to synthesize progestin hormones.
These changes in endocrine activities are accompanied by the resumption of meiosis and the maturation of the cytoplasm of the oocyte, and culminate in ovulation.