'Addison's disease
Diagnosis
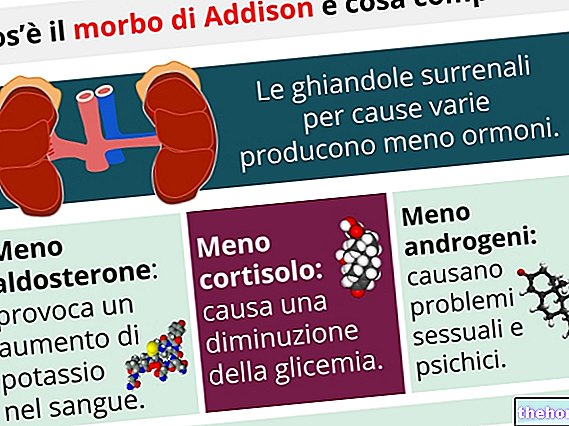
The diagnosis of Addison's disease is quite simple and is based on the blood dosage of sodium, potassium, cortisol, renin and ACTH (adrenocorticotropic hormone).In people with primary Addison's disease, plasma and urinary cortisol concentrations are quite low, while ACTH levels exceed the normal limit.
For the diagnosis of Addison's disease the following are indicative:
- low level of sodium in the blood (hyponatraemia);
- high level of potassium (hyperkalemia);
- high levels of ACTH and renin;
- insufficient cortisol response to the ACTH stimulation test.
Another important test is the ACTH stimulus test, during which cortisol levels in the blood and urine are measured before and after the injection of ACTH; in healthy people the stimulatory effect of the hormone translates into a consistent increase in serum cortisol levels; the same cannot be said for subjects with Addison's disease, where the intervention does not perform the expected action due to adrenal insufficiency. The same principle applies to the stimulus test for CRH, a hormone that favors the pituitary synthesis of ACTH; this test is therefore useful in evaluating secondary forms in which the pituitary gland secretes insufficient amounts of ACTH.
The doctor can also perform a CT scan or an abdominal magnetic resonance to evaluate any anatomical abnormalities of the adrenal glands and the hypothalamus-pituitary region, while a simple blood test can highlight the presence of specific antibodies against steroidogenesis.
Therapy
For further information: Drugs for the treatment of Addison's disease
Addison's disease is a chronic disease, as such subject to continuous drug treatment. After the diagnosis is established a replacement therapy able to replenish the missing hormones; even if the adrenal damage is irreversible, thanks to this intervention the Addisonian patient will be able to lead a practically normal life.
It is very important not to skip doses and to respect the intake times recommended by your doctor.
It is useful to carry a medical card or other means of identification with you to alert healthcare professionals of your illness in the event of an accident or when it is impossible to communicate. It is also advisable to carry a kit with the medicines to be taken in case of emergency. It is also advisable to have a cortisol-based preparation to be administered by injection, in case a pathology with vomiting prevents normal oral intake.
In the presence of acute adrenal insufficiency, if the patient is not promptly subjected to correct therapy with high dose intravenous or intramuscular cortisone, together with rehydrating and hyperglycemic infusion therapy, it can lead to coma or death.
By virtue of the hormones secreted by the adrenal gland, replacement therapy involves the administration of substances with glycoactive (glucocorticoids), mineralactive (mineralocorticoids) and, in women, weak androgens. In this sense, the main challenge for the endocrinologist is represented by the "identification of the drug and the appropriate therapeutic dose, which can vary from individual to individual and, in the same subject. In the different physiological conditions in which he finds himself. In particular circumstances stress, for example, it is necessary to intervene with higher pharmaceutical doses in order to avoid a serious addisoninan crisis.
The goal of treatment is to eliminate hormone deficiency symptoms without inducing excess symptoms, while maintaining a balance that does not expose the patient to the Addisonian crisis. By virtue of these considerations, individuals with Addison's disease must undergo regular and periodic checks throughout life: the adequacy of the replacement therapy is in fact established through laboratory tests, but also on the basis of the sense of well-being perceived by the patient. These checks (the most important is the dosage of free cortisol in the urine) are not particularly complex and above all do not create discomfort for those who have to perform them.
GLUCOCORTICOID THERAPY
In a normal subject, the daily production of cortisol is around 20 mg, with a circadian rhythm synchronized with the sleep-wake phases (maximums just before waking up and minimums in the late evening). On the basis of these physiological assumptions, in the patient suffering from Addison's disease, therapy with glycoactive substances is often divided into several doses; however, there are also long-acting glucocorticoids such as dexamethasone (Decadron) and prednisone (Deltacortene) which can be taken in a single administration, usually at bedtime.
In addisonine crises, the emergency treatment performed by the healthcare professional is based on the intravenous injection of glucose, saline and hydrocortisone. Generally this treatment allows a rapid recovery.
However, most of the time the replacement dose [hydrocortisone (Hydrocortone, plenadren) and cortisone acetate (Cortone)] is divided into three parts, two of which are taken in the morning and one in the afternoon (in order to mimic the physiological circadian just described).
MINERALCORTICOID THERAPY
It is not necessary in the secondary forms and is based on the intake of the corticosteroid 9α-fluorohydrocortisone. The doses of this drug must be adapted according to the mineralocorticoid power of the glycoactive drug used and once again in relation to the condition of the subject; in the hot months , especially in muggy environments or when practicing an intense sporting activity, for example, it is necessary to increase the doses to accentuate fluid retention and prevent dehydration.
ANDROGENIC THERAPY
In women with Addison's disease, a therapy with a weak androgen (DHEA or dehydroepiandrosterone) is often recommended in order to improve the sense of well-being and sexual vitality.
More articles on "Addison's disease: causes and treatment"
- Addison's disease
- Addison's disease - Drugs to treat Addison's disease













-non-sentire-gli-odori.jpg)