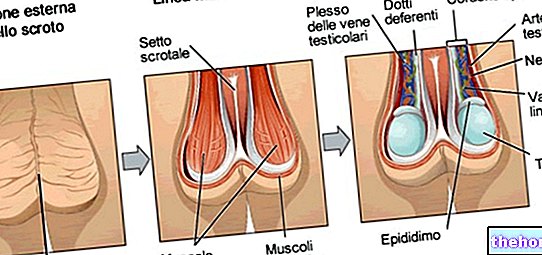
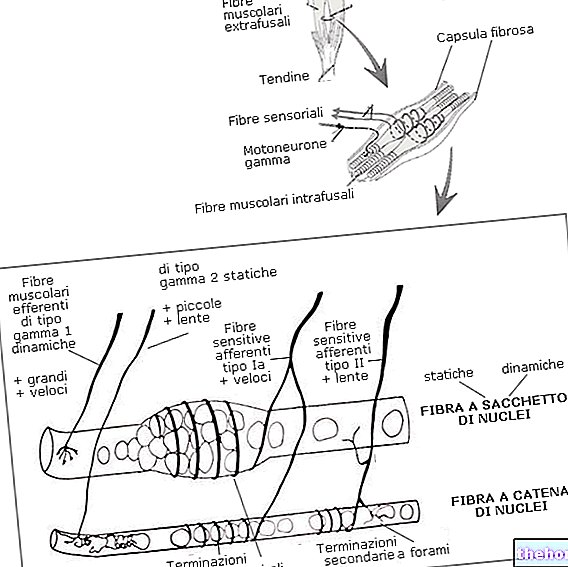
Symptoms and manifestations
As expressed several times in the article, diabetic nephropathy is a progressive disease, which passes through stages of increasing severity from total asymptomaticity to irreversible chronic renal failure.
STADIUM I
Defined as the stage of glomerular hyperfiltration, it is characterized by the absence of symptoms and by apparently normal renal function. In reality, histological alterations are also evident in this phase and it is possible to demonstrate the presence of
- polyuria, occasional glycosuria and a constant increase in glomerular filtrate, 20-50% higher than in healthy subjects of the same age; at this stage the urinary excretion of albumin is normal
STADIUM II
Also called "silent nephropathy"
- Also in this phase no symptoms are present, but, especially after physical exertion or food abuse, microalbuminuria appears. The term microalbuminuria was coined to report the urinary presence of albumin in modest but still significant concentrations from a chemical and clinical point of view.
STAGE III
Also known as the "incipient nephropathy" stage
- In this stage, microalbuminuria is permanent and occurs even in the absence of physical exertion or food abuse. The glomerular filtrate is reduced, but still remains at high values; arterial hypertension often appears
STADIUM IV
Also known as the "overt nephropathy" stage
- An overt proteinuria is found (> 200 µg / min), and the glomerular filtrate is reduced to frankly pathological values. Constant arterial hypertension, constant increase in blood creatinine. The transition from microalbuminuria to proteinuria also marks the transition of diabetic nephropathy from the pre-clinical to the clinical phase. Symptoms and complications are typical of nephrotic syndrome: edema, therefore swelling especially in the face, feet and abdomen, finding of foam in the urine, increased susceptibility to infections, malnutrition, increased cardiovascular risk (thrombosis and hyperlipidemia ), anemia, weakness, malaise.
STADIUM V
Also known as uremic stage or "Chronic renal failure"
- It is characterized by chronic renal failure which evolves towards terminal uremia which requires dialysis treatment. Diabetics tolerate uremia less than chronic uremics, so their survival is shorter.
Diagnostic criteria
Standard urinalysis is the first step in the diagnostic process and screening for diabetic nephropathy.
To be able to speak with confidence about diabetic nephropathy it is first of all necessary to exclude the numerous causes that can alter urinary albumin excretion: infections, but also decompensated diabetes (occasionally high hyperglycemia), physical activity, urinary infection, fever, heart failure and hypertension. Hence the need not to limit oneself to the dosage of albumin alone, but to extend the examination to the evaluation of other important parameters: urine sediment analysis, leukocyte count, glucose and nitrite dosage. .
- MICROALBUMINURIA:> 30 mg / day or 20 µg / min or 30 µg / mg creatinine
- PROTEINURIA OR MACROALBUMINURIA: albuminuria> 300 mg / day
PLEASE NOTE: The urinary excretion of albumin shows notable variations from day to day; for this reason, the certainty of being in front of a microalbuminuric patient is obtained only through the detection of high levels of albumin in at least 2 out of 3 samples collected over a period of 3-6 months.
Therapy and prevention
Preventive and therapeutic strategies to delay the onset of diabetic nephropathy and its evolution towards chronic renal failure include:
- Intensive (rigorous) blood glucose control, the target of which is represented by percentages of glycated hemoglobin lower than 6-7%, to be implemented through:
- dietary control (see diet and diabetes)
- regular physical activity (see sports and diabetes)
- drug therapy (see diabetes drugs)
- Control of arterial hypertension, whose target is represented by blood pressure values around 125/75 mmHg, to be implemented through:
- dietary control (see diet and hypertension)
- regular physical activity (see sport and hypertension)
- drug therapy to be implemented with ACE inhibitors, Angiotensin II receptor antagonists and / or sartans
- Restriction of caloric intake in case of overweight or obesity; in case of diabetic nephropathy the target is to maintain the BMI between 20 and 25
- Restriction of the protein intake in the diet (low protein diet) by favoring proteins of vegetable origin and fish, whose target is represented by a protein intake of 0.8 g / kg (about 10% of daily calories). dietary intervention is especially useful in tertiary prevention, to prevent or slow down the evolution of the disease from the stage of overt diabetic nephropathy to that of uremia
- Abolition of smoking
- Correction of dyslipidemia, whose target is represented by LDL values below 100 mg / 100 ml (see: drugs for high cholesterol)
- Abstention from nephrotoxic drugs (contrast agents, antibiotics and NSAIDs such as ibuprofen, naproxen and celecoxib)
Dialysis treatment is necessary for patients who have reached the fifth stage. The isolated kidney transplant or the joint kidney-pancreas transplant is almost always contraindicated in type 2 diabetics due to the presence of cardiovascular alterations and other risk factors (advanced age, poor life expectancy ...) that can compromise the outcome of the "intervention.
Other articles on "Diabetic Nephropathy: Symptoms and Therapy"
- Diabetic Nephropathy: Causes and Pathophysiology
- Diabetic nephropathy