Operative hysteroscopy requires special preparation, which also includes a series of tests aimed at establishing a woman's suitability for the procedure in question.
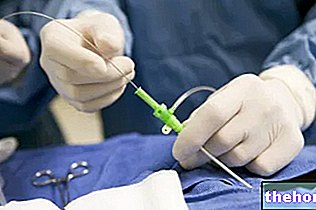
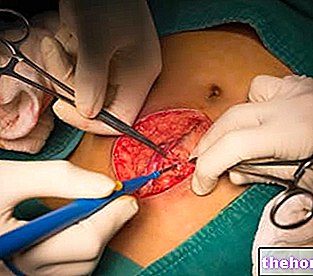
With a duration of 30-60 minutes, operative hysteroscopy involves the insertion into the uterine cavity, through the vaginal opening, of the hysteroscope, which acts as a surgical instrument.
Operative hysteroscopy is a safe and effective procedure, which, at its conclusion, requires a few days of rest pending complete recovery.
Brief review of what "is" Hysteroscopy
Hysteroscopy is an endoscopic gynecological procedure, which allows to evaluate from the inside the state of health of the uterus - in particular of the uterine cavity, cervical canal and endometrium - and, in case of need, to intervene surgically , in order to cure some medical condition.
Hysteroscopy is based on the use of an instrument known as a hysteroscope; the latter is a long tube, similar to a drinking straw, which, thanks to the equipment of a camera and a system for connecting to a monitor, acts as an exploratory probe of the uterus and cervix, after its insertion into the uterine cavity , through the vaginal opening.
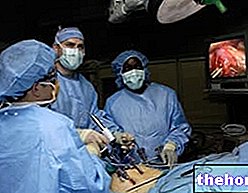
Hysteroscopy is a procedure usually performed on an outpatient or outpatient basis Day surgery; therefore, except in special cases, it never provides for the patient to be hospitalized.
Hysteroscopy is a subject for gynecologists, ie doctors with a specialization in gynecology.

Shutterstock
- The removal of benign tumors of the uterus other than uterine polyps and fibroids;
- Removal of intrauterine adhesions;
- The removal from the uterus of post-abortive placental residues (ie after an abortion) or post-partum (ie after a birth);
- The extraction of the so-called intrauterine system (or IUS), a particular device which, inserted in the uterus, acts as a temporary contraceptive;
- The realization of the so-called tubal sterilization, a form of permanent contraception. Tubal sterilization is also called tubal closure.
Health assessment tests
To establish suitability for operative hysteroscopy, the prospective patient must undergo:
- A "careful gynecological examination;
- An "accurate medical history (or clinical history). It includes a series of investigations, which serve to clarify important aspects such as: the past illnesses of the eligible patient and her family; any medications taken by the eligible patient at the time of checks; the habits of the patient. eligible patient (e.g. cigarette smoke); etc .;
- A cervicovaginal swab. It is used to establish whether a "cervical or vaginal infection is in progress;
- A "transvaginal ultrasound. Provides information on the anatomy and health of the pelvic organs, such as the vaginal canal, uterus, ovaries, and fallopian tubes;"
- Blood analysis. They are used to verify the presence or absence of any coagulation disorders;
- A pregnancy test. As will be seen later, pregnancy represents a contraindication to operative hysteroscopy.
Important note
The aforementioned examinations are also provided for in the case of possible diagnostic hysteroscopy.
On the day of the procedure: how to behave?
Remember that: at this stage of preparation, there is "suitability" for the operative hysteroscopy procedure.
On the day of the operative hysteroscopy, the patient must wear comfortable and practical clothes, because then she will have to remove them in favor of a hospital gown specially prepared for her by the medical staff.
How to behave if anesthesia is foreseen?
Under certain circumstances, operative hysteroscopy may require general anesthesia.
General anesthesia is an anesthetic practice which requires the observance of a fast of at least 8 hours and which provides for the patient to fall asleep and unconsciousness until the end of the surgical procedure, in order to make him insensitive to any pain or discomfort.
In the case of general anesthesia, then, it is necessary that a relative (or a trusted friend) of the patient makes himself available to take his loved one home, as the latter is not in the physical condition to drive a means of transport and take care 100% of himself (upon awakening from general anesthesia, in fact, for a few hours, confusion, slow reflexes, malaise, headache, etc. appear).
Did you know that ...
From a general anesthetic point of view, failure to comply with complete fasting involves the cancellation of the entire planned surgical procedure, even if all other circumstances exist to perform it.
, which, thanks to a speculum, opens the vagina and gently introduces the hysteroscope, in order to lead it into the uterine cavity.
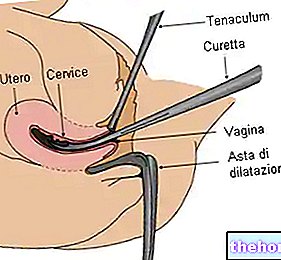
To more easily lead the hysteroscope inside the uterus, the gynecologist needs to stretch (in the sense of dilating) the walls of the uterine cervix, cervical canal and uterine cavity; during operative hysteroscopy procedures, this work distension is obtained with an "injection through a hysteroscope of a liquid substance, called" distension liquid ".
The hysteroscope is internally hollow to allow the passage of gases, liquids or thin surgical instruments.
The distension (or dilation) of the uterus is essential not only to facilitate the conduction of the hysteroscope inside the uterus, but also to allow a better view of the internal anatomy of the organ and to make the entire procedure less painful. .
In this phase of the procedure, it is important to carefully monitor the intrauterine pressure by the entire medical staff, which must remain at a value between 60 and 70 mmHg. Maintaining these blood pressure values, in fact, avoids the over-distension of the walls constituting the uterine cavity and prevents the diffusion into the abdomen, through the fallopian tubes, of the distension fluid.
SECOND PART
When the hysteroscope is finally inside the uterus and the uterus is sufficiently dilated, the gynecologist can start the planned treatment on the affected uterine area. Thanks to the hysteroscope camera (which is also equipped with a light source), the therapeutic action is very precise.
PART THREE
At the end of the therapeutic intervention, the gynecologist proceeds to gently extract the hysteroscope. With the extraction of the hysteroscope, the operative hysteroscopy can be said to be over.
Where is anesthesia placed, when it is foreseen?

In the above description of the various stages that characterize operative hysteroscopy, general anesthesia takes place after the patient has been accommodated, but before the insertion of the speculum and the hysteroscope.
Once administered, the anesthetics work within minutes.
Remember that general anesthesia causes the recipient to fall asleep, which lasts until the end of the procedure.
An anesthesiologist, that is a doctor specialized in anesthesia and resuscitation procedures, always provides for general anesthesia practices.
Instrumentation for Operative Hysteroscopy
The instrumentation for operative hysteroscopy includes: hysteroscope, speculum (vaginal valves), forceps, dilators, cannulae, insufflator, video camera system, sterile gauze, fiber optic cable, CO2 conductor cable, etc.
The preparation of this instrumentation - however obviously properly sterilized - takes place while the patient is wearing the gown provided for the procedure.
Did you know that ...
There are two types of hysteroscope: the hysteroscope for diagnostic hysteroscopy procedures, whose diameter is between 4 and 5 millimeters, and the hysteroscope for operative hysteroscopy procedures, whose diameter is 7-8 millimeters.
How do patients feel during an "Operative Hysteroscopy?"
Without the practice of anesthesia, the patient undergoing operative hysteroscopy may experience slight discomfort / pain during the introduction of the hysteroscope into the vagina and cervical canal. This sensation, however, is temporary, as readers will remember , the gynecologist follows the introduction of the hysteroscope by dilation of the uterine cervix and uterus.
With general anesthesia, however, the patient sleeps and is insensitive to pain for the entire duration of the operative hysteroscopy.
How long does the Operative Hysteroscopy last?
As a rule, an operative hysteroscopy procedure lasts 30-60 minutes.
The duration of an "operative hysteroscopy depends on the medical condition present and how easy it is or not to treat."
Did you know that ...
Diagnostic hysteroscopy lasts significantly less than operative hysteroscopy; its duration, in fact, generally does not exceed 15 minutes.
When is the return home after an "Operative Hysteroscopy?"
The patient undergoing operative hysteroscopy can return home only after a series of medical examinations, aimed at assessing the success of the procedure and the body's response to a "possible general anesthesia (eg: monitoring of vital functions, etc.) .
Normally, these medical examinations take from 2 to 4 hours, a period of time in which the patient receives all the necessary attention from the nursing staff.
Complications
By complications of a diagnostic or operative procedure, doctors mean problems of a certain clinical relevance, which can occur during or after the aforementioned procedure.
Potential complications of operative hysteroscopy procedures include:
- Uterine perforation;
- Bladder perforation;
- Development of a "pelvic infection (metritis);
- Tearing of the blood vessels of the uterus resulting in heavy vaginal bleeding;
- Endometritis, ie inflammation of the endometrium;
- Peritonitis, that is, inflammation of the peritoneum;
- Severe allergic reaction (anaphylactic shock) to anesthetics;
- Uterine edema;
- Gas embolism (related to the practice of general anesthesia);
- Trauma to the cervix caused by the hysteroscope.
How to recognize any complications?
The most classic symptoms of complications associated with operative hysteroscopy are:
- Intense and protracted abdominal pain that does not subside with the most common analgesics;
- Fever above 38 ° C;
- Heavy and recurrent vaginal bleeding;
- Leakage of dark, foul-smelling fluid from the vagina.

- Endometrial carcinoma;
- The pregnancy;
- Pelvic inflammatory states, such as endometritis, metritis, pelvic peritonitis, acute vaginitis and acute cervicitis.
Furthermore, doctors deem it unsuitable to perform diagnostic hysteroscopy in the case of: nulliparity, intact hymen and cervical stenosis.
Did you know that ...
The contraindications to operative hysteroscopy listed above also apply in the case of diagnostic hysteroscopy.