What is the hysterectomy
The hysterectomy is the surgery by which the uterus is removed.
Total or Partial?
We speak of a total hysterectomy when the operation leads to the removal of the entire organ, and of a partial or subtotal hysterectomy when the neck or cervix (tract that protrudes down into the vagina) is preserved.

Extension to other organs
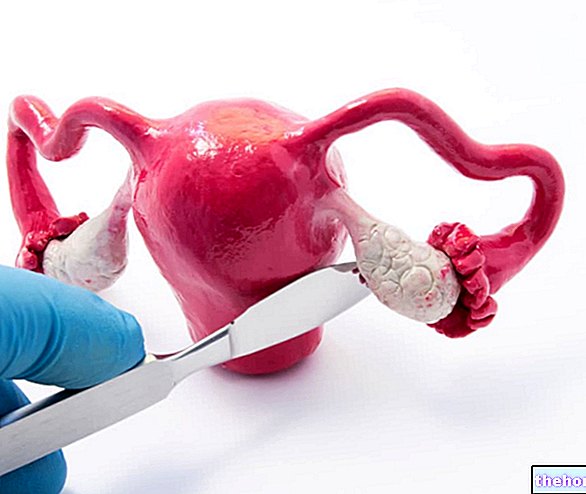
The hysterectomy operation can be extended to the ovaries, for example when it is necessary to remove them due to the presence of ovarian cysts, and to other contiguous anatomical structures, such as the uterine salpingi that connect the uterus to the ovaries (in this case the operation is called hysterosalpingectomy), the upper third of the vagina and the parametrium.
Consequences on Fertility and Sexuality
The hysterectomy forever compromises the possibility of having a pregnancy, while the surgical menopause is inevitable only when the operation has also included the removal of the ovaries.
In any case, the operation does not significantly affect either the desire or the sexual activity, even if the libido could be negatively influenced by the psychological implications of the intervention.
When is it needed?
The hysterectomy is only necessary in the presence of important problems, for which the operating room represents the safest and most effective solution; a malignant tumor (carcinoma) of the uterus, for example, but also a benign tumor form (fibroid), if it causes severe bleeding or compression phenomena in the lower part of the abdomen, triggering pain similar to renal colic.
In addition to these primary indications, surgery can also be performed to resolve severe endometriosis (growth of uterine lining outside the uterus) or excessive increase in menstrual flow (menorrhagia).
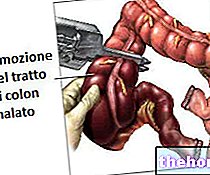
How is it done?
The techniques used by the surgeon can be different. They range from the classic and more invasive open hysterectomy surgery, in which a cut is made on the abdomen, to more innovative techniques, such as the vaginal one (blow-hysterectomy) in which the uterus is "removed" from the vagina, and laparoscopy.
This latest technique, which has positively revolutionized many surgical interventions, involves the insertion of micro-instruments through small incisions, guaranteeing rapid recovery after the operation.
Hormone Replacement Therapy
Surgical menopause induced before the natural one increases the typical problems of this period of life.
For this reason, also considering the lower risk of side effects and the greater severity of the disorders associated with it, hormone replacement therapy is often used.
By replacing the hormones produced by the ovary (estrogen), the risk of osteoporosis, cardiovascular disease and other minor problems is reduced. We must not forget that natural menopause is a slow and gradual process, which gives the body time to get used to hormonal changes and loss of endocrine function of the ovaries. If menopause is surgically induced, the body experiences this sudden endocrine shock more severely.
For women who have undergone hysterectomy, hormone replacement therapy is generally estrogen-only, since the protective effect of progestogens on the development of uterine endometrial cancer is not necessary.
If the hysterectomy is only partial (ovaries preserved) and performed at a young age, there is in any case a high risk of going against, over the years, a premature loss of ovarian function (early menopause), with consequent increase in the cardiovascular, osteoporotic risk and to accuse in a more severe way the typical ailments of this period (such as hot flashes).
Complications
Even if the hysterectomy is, at least in most cases, a decisive intervention (the cancers, for example, remain in the cervicouterine for a long time without spreading to other body regions), it is certainly not without important repercussions that involve both the physical sphere, as well as the psychic, social and affective one of the patient.
When the hysterectomy is total, the risk of vaginal prolapse increases, that is the danger that one or more pelvic structures, such as the bladder and rectum, descend downwards until they exit the vaginal intake. Finally, the psychological repercussions of the intervention, often harshly perceived as a loss of femininity, as well as fertility, should not be overlooked.






-cos-e-malattia-nelluomo.jpg)