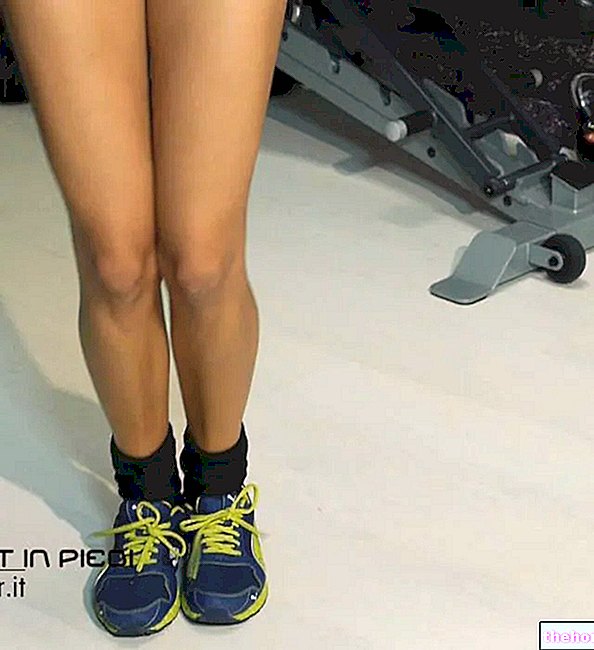This dangerous neurological condition can affect the white matter or the gray matter of the spinal cord, with the final unpleasant effect of altering the functions of the latter.
The causes of myelitis are numerous; these include: viral infections (including the well-known polio), bacterial infections (eg Lyme disease), fungal infections, parasitic infections, autoimmune diseases and some vaccination practices.
Symptoms of myelitis vary from patient to patient, depending on the underlying cause and involvement of the white matter or gray matter.
In order to plan an appropriate treatment against the consequences of myelitis, a precise diagnosis of the causal factor is essential; this explains why the diagnostic process always includes various investigations (neurological examination, radiological examinations, lumbar puncture, etc.).
Brief Review of the Spinal Cord?
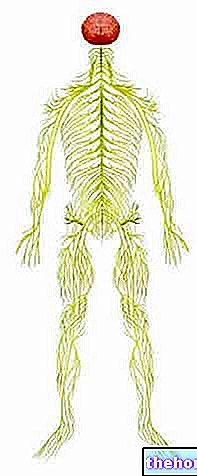
The spinal cord is, together with the brain, one of the two fundamental components of the central nervous system.
Structurally very complex, this vital nervous organ has several groups of neurons (arranged in white matter and gray matter) and 31 pairs of nerves (the so-called spinal nerves), and has the important task of sorting the incoming and outgoing signals between the different brain areas (lobes of the brain, cerebellum, etc.) and the rest of the organism.
The spinal cord takes place, in order to receive protection, inside the so-called spinal canal, that is the duct resulting from the overlapping of the vertebrae of the spinal column and their characteristic holes.
What does myelitis involve? The main consequences
The correct functioning of the spinal cord depends on the good health of each of its constituent parts.
The inflammation produced by myelitis is potentially capable of damaging the neurons of the gray matter or white matter and this has, as a consequence, the non-fulfillment, by the spinal cord, of the vital process of sorting the nerve signals between the various areas cerebral and the rest of the organism.
Myelite: origin of the name
The term "myelitis" is the result of the "union of the words" mielo ", which refers to the spinal cord, and" ite ", which in medicine is the suffix indicating inflammatory processes.
, autoimmune diseases and some vaccines.
Myelitis and Bacteria
The best known bacteria capable of causing myelitis are:
- The tuberculosis bacterium (Mycobacterium tuberculosis);
- The bacterium responsible for Lyme disease (Borrelia burgdorferi);
- The syphilis bacterium (Treponema pallidum);
- Bacteria that cause meningitis (Meningococcus, Pneumococcus and Haemophilus influenzae type B).
In general, it is very rare that a form of myelitis can result from a "bacterial infection."
Myelitis and Viruses
Viruses related to the onset of myelitis include:
- The poliovirus. It's the polio virus. It has a direct action on the spinal cord, in that, in causing myelitis, it specifically affects the neurons of the medullary gray matter;
- Herpes zoster virus, varicella virus, HIV virus (or AIDS virus), some enteroviruses and flaviviruses (eg West Nile virus and Japanese encephalitis virus). These viruses can directly cause myelitis, as they are capable of penetrating and infecting the neurons of the spinal cord;

- Some viruses of the respiratory tract and gastrointestinal tract. Any myelitis resulting from these viruses usually appears at the end of the infection.
Myelite and Fungi
The fungi that cause myelitis are those capable of infecting the bones of the spinal column (vertebrae) and forming on these abscesses or granulomas; these formations, in fact, produce a compression of the spinal cord, contained in the spinal canal, with inflammatory results.
Specifically, in the list of fungal pathogens related to myelitis, take part:
- Cryptococcus neoformans;
- Coccidioides immitis;
- Blastomyces dermatitidis;
- Histoplasma capsulatum;
- Some species of Candida;
- Some species of Aspergillus;
- Some zygomycetes.
Myelitis and Parasites
The parasites responsible for myelitis are those which, in particular larval forms, are able to penetrate the cells of the central nervous system, including the neurons of the spinal cord.
In detail, among the parasites capable of producing myelitis, there are:
- Some species of Schistosoma;
- Toxocara canis;
- Some species of Echinococcus;
- Taenia solium;
- Trichinella spiralis;
- Some species of Plasmodium.
Myelitis and Autoimmune Diseases
Autoimmune diseases are pathologies in which the immune system of an organism, instead of protecting the latter, attacks it through improper and exaggerated responses.
In myelitis caused by an autoimmune disease, inflammation of the spinal cord is the result of the improper aggression that the immune system exerts on neurons of the white or gray matter.
Among the autoimmune diseases capable of producing myelitis, the following deserve a mention: systemic lupus erythematosus (SLE), multiple sclerosis, Sjogren's syndrome and optic neuromyelitis (or Devic's disease).
Myelitis and Vaccines
Vaccines that, in rare circumstances, can cause myelitis include:
- The hepatitis B vaccine;
- The measles, mumps and rubella vaccine;
- The tetanus and diphtheria vaccine.
Types of Myelitis
Experts recognize the existence of at least 4 types of myelitis based on the causes and localization area of the inflammation on the spinal cord.
These 4 types of myelitis are:
- Polio. This typology includes all forms of myelitis that affect the gray matter neurons of the spinal cord.
Usually, it is connected to the aforementioned poliovirus (which motivates its name); however, it can also arise as a result of infections sustained by other viruses, such as some echoviruses, coxsackieviruses and enteroviruses.
Polio is also known as gray matter myelitis. - Leukomyelitis. This type includes all forms of myelitis characterized by a lesion of the white matter neurons of the spinal cord.
- Transverse myelitis. This typology includes all forms of myelitis affecting the white matter in which the inflammation extends over the entire width of a more or less significant tract of the spinal cord.
- Meningococcal myelitis (or meningomyelitis). This type includes all forms of myelitis in which there is also an "inflammation of the meninges of the spinal cord.
Outline of Pathophysiology: What Does Myelitis Cause?
In myelitis, damage to the spinal cord affects axons devoid of myelin, in the case of gray matter neurons, and myelin, in the case of white matter neurons.
and stiffness in the neck, back and / or extremities (limbs);Did you know that ...
Pain induced by a neurological disease such as myelitis is an example of neuropathic pain.
In medicine, the term "neuropathic pain" refers to the painful sensation that appears as a result of the deterioration or malfunction of the neurons of the central and / or peripheral nervous system.
Symptoms of Poliomyelitis and Transverse Myelitis
This section is devoted to the symptoms of the two most important forms of myelitis: polio and transverse myelitis.
In polio, the typical symptom picture includes: fever, headache, nausea, widespread fatigue, pain and stiffness in the neck, back and extremities, muscle spasms, flaccid paralysis, vomiting, tingling in various parts of the body, atrophy muscle and cardiovascular problems (in severe cases).

In transverse myelitis, on the other hand, the characteristic symptoms include: back pain, paraesthesia in the hands and feet, paralysis of the limbs, a sense of weakness in the arms and legs, urinary incontinence, fecal incontinence, difficulty urinating, constipation, loss of appetite, spasms muscle and sharp pains in the arms, legs, chest and abdomen.
Symptoms of myelitis: how long does it take to appear?
Typical symptoms of myelitis appear over hours to a few days and gradually worsen over a week or two.
For example, in the case of transverse myelitis, the characteristic symptom picture sets in within a few hours and reaches its peak of severity within 10 days of the onset of the condition.
Complications
In the absence of adequate treatment and in the most severe cases, myelitis can irreversibly damage the spinal cord and lead to complications such as:
- Chronic pain. Neck pain, back pain and pain in the limbs become chronic.
The chronicity of pain is highly debilitating for the patient, because it makes it difficult to carry out numerous daily activities, even the simplest. - Muscle spasms more and more frequent. As with chronic pain, the increased frequency of muscle spasms is also an obstacle to daily activities.
- Total paralysis of arms and / or legs. It drastically limits the daily needs of patients.
- Sexual dysfunctions. For men, they basically consist of erectile dysfunction; for women, on the other hand, in anorgasmia (absence of orgasm).
- Depression. It is the result of the previous complications; after all, the patient does not enjoy moments of respite from pain, finds it impossible to carry out even very simple activities and is no longer able to fully live his own sexuality.
- Severe cardiovascular problems. They are possible in the presence of severe forms of myelitis; can cause death of the patient.
Report of symptoms, physical examination and anamnesis
- The description of the symptoms is very important for diagnostic purposes, because it allows the doctor to know in detail the precise suffering of the patient.
- The physical examination and the anamnesis serve to further clarify the symptomatological picture and to identify the possible causal factors of the condition in progress.
Neurological visit
A thorough neurological examination serves to establish the patient's neurological health.
It is a "survey that includes various tests to evaluate the functionality of the nerves.
Radiological examinations
The magnetic resonance and the CT scan of the spine provide very detailed images of the latter and the spinal cord, so they are able to identify any abnormalities or alterations (eg: granulomas or abscesses induced by some fungus).
Radiological examinations are also useful for the purpose of the so-called differential diagnosis (ie the diagnostic approach that allows to identify a pathology by proceeding by exclusion).
Lumbar puncture
The lumbar puncture consists in taking some cephalorachidian fluid from the spinal canal of the spinal column and in its subsequent laboratory analysis. It is a fundamental test to detect the presence of infectious agents in the spinal cord (and in the nervous system in general. ) and to understand if there is a "local inflammation".
In a suspected case of myelitis, rachycentesis allows the diagnostic doctor to determine if there is "indeed" inflammation in progress and if that inflammation is due to a certain pathogen.
Blood analysis
In a context of myelitis, blood tests can help determine whether the condition is caused by pathogens or by abnormal behavior of the immune system (e.g. in those suffering from optic neuromyelitis, they allow to identify the typical antibodies responsible for the condition).
Why is it important to identify the causes of myelitis?
The knowledge of the causes of myelitis is very important, because it is on the causal factors that the planning of the most adequate therapy depends.
intravenously. Cortisones are anti-inflammatory drugs; therefore, in the presence of myelitis they serve to reduce inflammation of the spinal cord;Alternative treatment to the intravenous administration of cortisone, it is used in the presence of autoimmune myelitis.