«Coombs Test in Pregnancy
Prophylaxis of haemolytic disease of the newborn
What is the anti-Rh prophylaxis?
The possibility of preventing Rh immunization through anti-D immunoprophylaxis represents a milestone in the history of medicine.
Anti-D prophylaxis is based on the intramuscular injection of anti-D (anti Rh) immunoglobulins on the shoulder. In the Rh negative mother

In addition to the moment of delivery, the prophylaxis of haemolytic disease of the newborn is also performed in the case of:
- threat of abortion with blood loss;
- spontaneous or voluntary abortion (except for those that occur before the 13th week);
- abdominal trauma;
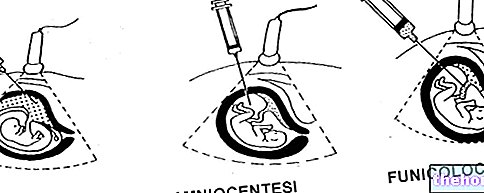
- villocentesis, amniocentesis and cordocentesis (funiculocentesis).
It may be prudent to perform anti-D immunoprophylaxis even in the case of:
- ectopic pregnancy;
- threat of abortion;
- blood loss;
- death of the fetus;
- obstetric procedures such as maneuvers for the cephalic version.
To prevent the disease, it is essential that prophylaxis is carried out promptly, within 72 hours of delivery or of the other potentially sensitizing events listed above.
In order to prevent any form of anti-D immunization during the course of pregnancy, for example due to an abnormal passage of red blood cells from the fetal to the maternal cardiovascular system, anti-D prophylaxis can be performed on all Rh negative women during the first pregnancy. This further reduces the risk of developing anti-D antibodies during gestation.
In very rare situations, the administration of anti-D immunoglobulins could cause serious maternal immunological reactions and, although the products used are highly controlled, the possibility (in any case very remote) of transmission of viral infectious diseases cannot be completely excluded.
INTRAUTERINE TRANSFUSION
In cases where, for various reasons, it has not been possible to initiate a prophylaxis with anti-D immunoglobulins, when the gravity of the circumstances requires it, doctors can resort to an early transfusion of fetal blood into the uterus, in order to make it similar to that of the mother. After birth, the transfused blood will gradually be replaced by that produced in the baby's bone marrow.
Unfortunately, intrauterine intravascular transfusion, that is carried out directly into the umbilical vein, is a practice that is not free from serious complications; therefore it should only be performed by expert personnel, in specialized centers.
Coombs test, blood group and haemolytic disease of the newborn
AB0 incompatibility: possible consequences
During pregnancy, immunization for blood groups A and B is even more frequent than Rh immunization, but unlike the latter, it rarely causes significant clinical problems. It affects about one percent of births, but only in "1.5 - 2% of cases there are important manifestations, such as to involve the need for transfusion therapy in 0.02% of cases.
In the case of a mother with a type 0 blood group and a father with a non-0 blood group, the baby may have AB0 incompatibility jaundice at birth, a condition that is usually not serious. As a rule, in fact, it is a jaundice not so high as to cause neurological problems and the anemia does not reach values such as to require blood transfusion. However, at birth, it will be necessary to carefully monitor both the bilirubin values and those of hemoglobin and hematocrit .
There is currently no preventive therapy for AB0 incompatibility.
Coombs Test, Summary and Key Points
- Hemolytic disease of the newborn is caused by the incompatibility between fetal and maternal blood, in which there are antibodies directed against the red blood cells of the fetus.
- The appearance of these antibodies is directed against particular antigens, the most common of which is the Rh factor (or D antigen), which is present in all subjects with Rh positive blood group. It is however possible, even if rare, to record the presence of antibodies directed towards other antigens (eg anti-Kell, anti-c, anti-E, etc.).
- For this reason, at the beginning of pregnancy all women undergo specific tests to establish the blood group and highlight the presence of free antibodies against red blood cells; these include the indirect Coombs test, which evaluates the presence of free antibodies against red blood cells.
- When the mother is Rh negative, it is necessary to know the blood type of the father, since the Rh factor is a dominant trait. If the father is Rh positive, the fetus will most likely also have the D antigen on its erythrocytes, resulting in a Rh incompatibility between mother and fetus. However, there is no problem when both partners are Rh negative, or if the mother is Rh positive and the father Rh negative.
- When the mother is Rh negative, the indirect Coombs test is repeated every month, while if the mother is Rh positive it is repeated in the third trimester of pregnancy.
- During gestation, thanks to the placenta, the maternal and fetal blood circulation remain well separated, so it is rare that significant antibody production is achieved against Rh positive fetal red blood cells. However, the problem recurs in the next pregnancy, or directly in the current one if for some reason the mother is already immunized against the D antigen (eg for previous blood transfusions, mixed use of syringes, etc.). once in contact with the antigen, the organism acquires and retains the ability to produce specific antibodies against this molecule. If the production of anti-Rh antibodies is already active, they cross the placenta, destroying fetal red blood cells.
- During pregnancy, the passage of fetal blood into the maternal circulation can occur during diagnostic procedures such as amniocentesis, CVS, cordocentesis, or even for a transfusion or abortion. Generally, therefore, in the case of Rh negative pregnant women an invasive diagnostic procedure, such as chorionic villus sampling or amniocentesis, is routinely subjected to treatment with anti-D immunoglobulins, which eliminate fetal red blood cells or block their antigenic sites.
- Anti-D immunoglobulin prophylaxis should be performed within 72 hours of delivery or of any other potentially sensitizing event (abortion, ectopic pregnancy, amniocentesis, CVS, etc.).
- To avoid sensitization already during pregnancy, for example due to small transplacental haemorrhages, immunoprophylaxis can be performed systemically at the 28th - 30th week of gestation, extending it to all Rh negative women. prophylaxis for forms of alloimmunization due to other antigens, the most frequent of which are anti-c and anti-Kell.