Generally, candida in pregnancy is not considered a "serious infection, however, in order to avoid complications, it should not be underestimated in any way and requires adequate treatment."
The symptoms of candida in pregnancy are similar to those that occur in non-pregnant women and are usually easily recognizable. In any case, it is always good to contact your doctor or your trusted gynecologist, in order to identify precisely which pathogen gave rise to the infection.
sustained by yeasts belonging to the genus Candida. In the majority of patients, the infection is triggered by the Candida albicans (80-95% of cases), infections caused by Hairless candida (5% of cases).
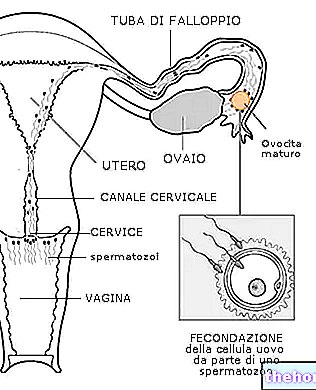
In many individuals, the Candida albicans it is normally present as a commensal in various parts of the body, including the vaginal mucosa in women. Generally, the yeast in question does not cause damage or pathologies, as it is kept under control by the pH and by the vaginal bacterial flora and by the body's defense mechanisms. However, in particular conditions, this control may fail and C. albicans it can proliferate excessively giving rise to the so-called candidiasis. When infections are localized in the female genitalia, it is usually referred to as vulvovaginal candidiasis.
(phenomenon that typically occurs during gestation);Among the risk factors that can contribute, favor or worsen infections and the manifestations of candida in pregnancy, we find:
- High blood sugar and diabetes (these two factors can favor the development of vaginal candidiasis in both pregnant and non-pregnant women);
- Excessive consumption of sugars;
- Any antibiotic therapies in progress;
- Use of underwear made of synthetic material;
- Cleaning and intimate hygiene not done correctly;
- Stress.
In truth, most of the aforementioned symptoms can also be caused by vaginal infections of different origins, for this reason, it is always good to contact your doctor or gynecologist who will be able to make a correct diagnosis of the disorder that afflicts the pregnant woman.
, the patient with candida in pregnancy shows caseous white plaques in the vaginal mucosa. The latter, moreover, appears edematous due to the ongoing infection.
The diagnosis can then be confirmed by "microscopic examination of the whitish vaginal discharge which will be able to accurately determine the presence or absence of Candida spp.
The execution of a correct diagnosis of candida in pregnancy is essential to undertake the most suitable treatment and to exclude the presence of infections or other diseases (for example, bacterial vaginosis or diseases caused by sexually transmitted pathogens, such as Chlamydia trachomatis or Trichomonas vaginalis).
- however, it must be adequately treated. Unfortunately, not all drugs usually used to treat this infection are also usable during the gestation phase.
However, it appears that topical imidazole-type antifungals can be used fairly safely during pregnancy. These drugs are generally formulated as creams or pessaries that must be applied directly to the vaginal level following the directions provided by the doctor (generally, once a day, in the evening before bedtime, for a period of at least 7 days). Miconazole and clotrimazole are the active ingredients most used to fight this fungal infection during pregnancy.
These drugs are considered safe because the local use of pharmaceutical formulations of this type gives rise to a reduced systemic absorption compared to other routes of administration, thus minimizing the potential risks for the fetus. However, as a precaution, the administration of these drugs it is not recommended during the first trimester of gestation.
The use of oral antifungals (such as, for example, fluconazole) is, on the other hand, generally not recommended due to the greater systemic absorption of the active ingredient and the potential damage that this could cause to the fetus.
In any case, all the aforementioned drugs can be used to combat candida in pregnancy only and exclusively if expressly prescribed by the doctor or gynecologist and only in cases where these health professionals deem it absolutely necessary and indispensable. The do-it-yourself treatment of fungal infections must not be carried out under any circumstances, especially if the infection with Candida spp. affects pregnant women.
, an action which, moreover, should be carried out regardless of the risk of encountering candida in pregnancy;If despite the adoption of the aforementioned precautions the candida in pregnancy should still present itself or worsen, a new medical consultation is absolutely essential.