Generality
Astrocytoma is a brain tumor that originates from particular cells of the glia, called astrocytes.
Astrocytomas can be benign or malignant and can have different growth powers.

Only thanks to an accurate diagnosis - through which the position and severity of the astrocytoma are outlined - is it possible to plan the most correct therapy.
Generally, the most suitable treatment, which offers the best chance of recovery, is surgical excision.
Brief reminder of brain tumors
When we talk about brain tumors, or brain tumors or brain neoplasms, we are referring to benign or malignant masses of cancer cells affecting the brain (hence an area between the telencephalon, diencephalon, cerebellum and brain stem) or the spinal cord . Together, the brain and spinal cord form the central nervous system (CNS).
The result of genetic mutations, the exact cause of which is not known very often, brain tumors can:
- originate directly from a cell of the central nervous system (in this case we also speak of primary brain tumors);
- derive from a malignant tumor present in other locations in the body, such as the breast (in this second case they are also called secondary brain tumors).
Given the extreme complexity of the central nervous system and the large number of different cells that compose it, there are many different types of brain tumors: according to the latest estimates, between 120 and 130.
Regardless of their malignancy or not, brain tumors must almost always be removed and / or treated with radiotherapy and / or chemotherapy, as they often cause neurological problems incompatible with a normal life.
What is astrocytoma?
Astrocytoma is a brain tumor that originates from particular cells called astrocytes.
Astrocytes are cells of the glia, therefore astrocytomas fall into the category of so-called gliomas, or brain tumors that arise from the cellular units of the glia.
An astrocytoma can be benign or malignant in nature; moreover, it can be focal or diffuse: focal astrocytomas appear as a mass of cells in their own right, distinct from the surrounding healthy brain tissue; diffuse astrocytomas, on the other hand, have the appearance of something "dispersed" in what surrounds them.

Difference between a benign tumor and a malignant tumor
A benign tumor is a mass of abnormal cells that grows slowly, has little infiltrative power and an "equally poor (if any) metastasizing power."
On the contrary, a malignant tumor is an abnormal cell mass that grows quickly, has a high infiltrative power and almost always a high metastasizing power.
NB: by infiltrative power, s "means the ability to affect adjacent anatomical regions. With metastatic power, on the other hand, we refer to the ability of tumor cells to spread, through the blood or the lymphatic circulation, to other organs and tissues of the body (metastasis).
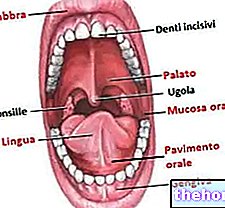
GLIA AND GLIA CELLS
With its cells, the glia provides support, stability and nourishment to the intricate network of neurons present within the human body and which have the task of transmitting nerve signals.
In the central nervous system, the cellular elements of glia are astrocytes, oligodendrocytes, ependymal cells and microglia cells.
In the peripheral nervous system (PNS), the cellular elements of the glia are Schwann cells and satellite cells.
LOCALIZATION OF ASTROCYTOMES
Astrocytomas usually form in the telencephalon, cerebellum, and brain stem.
Only in rare cases do they arise from an astrocyte located in the spinal cord.
ASTROCYTOMA: FROM GRADE TO DIFFERENT TYPES
Brain tumors are divided into 4 degrees - identified with the first four Roman numerals - according to their growth power.
Grade I and II brain tumors grow very slowly and involve a "small area of the brain; they are usually benign."
Conversely, grade III and IV brain neoplasms rapidly expand and invade surrounding tissue regions; they are generally malignant in nature.
A grade I or II brain tumor can, over time, turn into a grade III or IV tumor.
Based on the degree (or growth power) that characterizes them, astrocytomas are divided into:
- Pilocytic astrocytomas, which are grade I astrocytomas.
Features: are focal benign tumors, similar to fluid-filled cysts. - Diffuse low-grade astrocytomas, which are grade II astrocytomas.
Features: are widespread benign tumors. - Anaplastic astrocytomas, which are grade III astrocytomas.
Features: highly malignant tumors, they are called anaplastic because the astrocytes of the tumor mass lose their typical appearance and take on the characteristics of undifferentiated cells (process of anaplasia). - Multiform glioblastomas, which are grade IV astrocytomas.
Features: they are highly malignant and have a very high mortality. In the masses that constitute them, blood vessels, calcium deposits and cystic material can be found.
EPIDEMIOLOGY
Astrocytomas are the most common gliomas (N.B: gliomas are the most common brain tumors) and represent a third (therefore about 33%) of all primary brain tumors.
People of any age can develop an astrocytoma.
In children, slow-growing grade I astrocytomas are more common; in adults and the elderly, grade II and rapidly growing (grade III and IV) astrocytomas are more common.
Epidemiological features
Pilocytic astrocytoma
Pilocytic astrocytomas make up 2% of all astrocytomas.
Diffuse low-grade astrocytoma
Diffuse low-grade astrocytomas account for 8% of all astrocytomas, mainly affecting people between the ages of 30 and 40.
Anaplastic astrocytoma
Anaplastic astrocytomas make up 20% of all astrocytomas and mainly affect individuals between the ages of 30 and 50, and the elderly.
Glioblastoma multiforme
Multiform glioblastomas make up 15-17% of all primary brain tumors and 54% of all gliomas. They are the most common malignant brain neoplasms and particularly affect people aged 45 and over.
Causes
Astrocytomas, like almost all human brain tumors, arise for reasons that are not yet known.
Symptoms and Complications
The symptoms of an astrocytoma can appear suddenly or very slowly, depending on the growth that characterizes the tumor mass.
In other words, if the astrocytoma is grade I or II, the pathological manifestations start gradually; if, on the other hand, the astrocytoma is grade III or IV, the problems related to it appear and evolve very rapidly.
Although the site of tumor onset strongly affects the quality of symptoms, there are some symptoms common to almost all forms of astrocytoma, namely:
- Headache;
- Nausea and vomiting, especially in the morning;
- Poor eyesight;
- Seizures.
These disorders are due to the "increase in intracranial (or intracranial) pressure, which can occur for two reasons:
- Because the growing tumor mass prevents the cerebrospinal fluid from flowing normally.
- Because edema forms around the tumor mass.
HOW THE LOCATION OF THE CANCER AFFECTS THE SYMPTOMS
If the astrocytoma resides in the frontal lobe of the brain, patients tend to experience:
- Sudden or gradual changes in mood and personality
- Weakness or numbness in either side of the body
If the astrocytoma resides in the temporal lobe of the brain, the typical symptoms consist of:
- Problems with coordination
- Speech problems
- Memory impairment
Finally, if the astrocytoma resides in the parietal lobe of the brain, sufferers complain:
- Problems with writing
- Weakness or numbness in either side of the body
COMPLICATIONS
As far as malignant astrocytomas are concerned, the most serious complications are the "expansion of the tumor mass - which invades the surrounding healthy tissues - and the spread of neoplastic cells to other organs of the body (metastases).
As for benign astrocytomas, a possible complication is their change to malignant tumors.
Diagnosis
When faced with a suspected case of astrocytoma, doctors begin their diagnostic investigations with a thorough physical examination and an "analysis of the quality of tendon reflexes."

Finally, to dispel any doubts and to know the exact location and size of the tumor, they resort to specific tests such as:
- Nuclear magnetic resonance
- CT scan (or computed axial tomography)
- Biopsy of the tumor
- Lumbar puncture
OBJECTIVE AND TENDON REFLEX EXAMINATION, EYE TEST AND MENTAL-COGNITIVE EVALUATION
- The physical examination consists in the analysis of the symptoms and signs, reported or manifested by the patient. Although it does not provide any certain data, it can be very useful for understanding the type of pathology in progress.
- The examination of tendon reflexes is a test that serves to assess the presence or absence of neuromuscular and coordinative disorders.
- Using an eye test, the doctor observes the optic nerve and analyzes its involvement.
- The assessment of mental status and cognitive abilities is carried out with the aim of understanding which area of the central nervous system may have developed a neoplasm. For example, experiencing memory disturbances would tend to suggest a neurological problem based in the temporal lobes. , rather than in the parietal lobes and so on.
NUCLEAR MAGNETIC RESONANCE (NMR)
The nuclear magnetic resonance (NMR) is a painless diagnostic test, which allows to visualize the internal structures of the human body without the use of ionizing radiation (X-rays).
Its operating principle is quite complex and is based on the creation of magnetic fields, which emit signals capable of being transformed into images by a detector.
MRI scans of the brain and medulla provide a satisfactory view of these two compartments. However, in some cases, a venous injection of a contrast fluid may be necessary to improve the quality of the visualization. In such situations, the test becomes minimally invasive, because the contrast fluid (or medium) could have side effects.
A classic nuclear magnetic resonance scan takes about 30-40 minutes.
CT scan
CT is a diagnostic procedure that uses ionizing radiation to create a highly detailed "three-dimensional" image of the body's internal organs.
Although it is painless, it is considered invasive due to exposure to X-rays (NB: the doses of which are by no means negligible when compared to a normal X-ray). Furthermore, like MRI, it may require the use of a contrast agent. - not free from possible side effects - in order to improve the quality of the visualization.
A classic CT scan takes about 30-40 minutes.
BIOPSY
A tumor biopsy consists in taking and histological analysis, in the laboratory, of a sample of cells from the neoplastic mass. It is the most suitable examination if you want to trace the exact nature (benign or malignant) and severity of a tumor. .
In the case of an astrocytoma, the sampling is usually done during a CT scan - this allows for highly accurate sampling - and requires a small but delicate head surgery.
Treatment
The treatment to be adopted in the case of astrocytoma depends on numerous factors, including the degree, location, size and speed of growth of the tumor mass.
If the tumor resides in a position accessible to the surgeon's hands, the best thing to do would be to remove it. This is true both in the presence of a malignant neoplasm and in the presence of a benign neoplasm.
If the astrocytoma is malignant and / or widespread, radiotherapy and, sometimes, even chemotherapy must follow the surgical removal.
Treatment
I (pilocytic astrocytoma)
Surgical removal is generally the only treatment adopted and sufficient to cure the tumor.
II (diffuse low-grade astrocytoma)
Surgical removal and, if the diagnostic images show a significant dispersion of the tumor mass, also radiotherapy are needed.
III (anaplastic astrocytoma)
Surgical removal and radiotherapy are fundamental. In some situations (for example relapses), chemotherapy could also become so.
IV (glioblastomas multiforme)
SURGERY
The ultimate goal of the surgery is to remove all of the astrocytoma or, if this is impossible, most of the tumor mass.
The success of the removal depends on at least two factors, previously mentioned:
- The accessible or non-accessible location of the tumor mass. If the tumor is in an inaccessible location, it is impossible to remove it.
- The dispersion of the tumor mass into the remaining healthy brain mass. In this sense, grade I astrocytomas, which are focal, are easily removable.
Since the surgery is quite delicate and dangerous, the attending physician, together with his staff, is required to inform the patient of the possible risks of the procedure before it is performed.
RADIOTHERAPY
Tumor radiotherapy is a treatment method based on the use of high-energy ionizing radiation, with the aim of destroying neoplastic cells.
In the case of astrocytoma, it is adopted in two very different situations:
- After and upon completion of surgical interventions on grade II or higher astrocytomas.
- When the tumor is not surgically removable. In these situations, radiotherapy becomes the first and most important therapeutic treatment (N.B: this also applies to cases of pilocytic astrocytoma).
CHEMOTHERAPY
Chemotherapy is the administration of drugs capable of killing all rapidly growing cells, including cancer cells.
In the case of astrocytoma, doctors adopt it when they believe that the risk of a relapse (or recurrence) is high or when they believe that the tumor has spread some of its cells to the rest of the body (metastasis). Such situations are more likely when dealing with grade III or IV malignancies.
OTHER CARE
If the astrocytoma is causing edema around it, doctors may also plan corticosteroid therapy.
Corticosteroids are powerful anti-inflammatories, which are drugs that reduce inflammation.
Main side effects of radiotherapy
Main side effects of chemotherapy
Main side effects of corticosteroids
Tiredness
Itching
Hair loss
Nausea
He retched
Hair loss
Sense of fatigue
Infection vulnerability
Osteoporosis
Obesity
Indigestion
Hypertension
Agitation
Sleep disorders
OPERATIVE PHASE
After the surgical removal of the tumor and during any radiotherapy and chemotherapy treatments, the patient must also undergo physiotherapy rehabilitation.
The "objective of the latter" is to recover, at least in part, the neurological faculties (coordination, language, etc.) that the presence of the tumor mass or the intervention itself have compromised.
Prognosis
Prognosis mainly depends on three factors:
- By the degree of astrocytoma. After removal of a grade I astrocytoma, those affected have a good chance of making a complete recovery. more than 30 weeks.
- From the location of the neoplasm. The more the tumor mass is in an uncomfortable position for the surgeon, the more difficult it is to remove it. Failure to surgically remove the astrocytoma results in a drastic reduction in the survival rate, as radiotherapy and chemotherapy are not as effective.
- Since the diagnosis was made. The later the tumor is identified, especially if it is malignant, the lower the chances of recovery. Removal of the astrocytoma itself is less effective.