In detail, it is an acute infectious disease triggered by group A beta-haemolytic streptococcus.
Usually the infection affects children in pediatric age, while it rarely affects adults. Unfortunately, however, in some cases, scarlet fever can also occur in the latter and in pregnant women, giving rise to many concerns, especially as regards health. of the fetus.
In the course of the article, therefore, will be described the main characteristics of scarlet fever in pregnancy and the possible risks it can face when it is contracted by future mothers.
is rarely contracted, this possibility cannot be completely ruled out.
Fortunately, scarlet fever in pregnancy - in addition to occurring in rather rare cases - does not cause malformations in the fetus and, if promptly treated, should not cause harm of any kind.
, a Gram-positive coconut that can give rise to infections of various kinds. More precisely, the disease can be caused by strains of S. pyogenes of different types. For this reason, after the first infection there is no guarantee of "permanent immunity. Therefore, if a patient has contracted the disease once in her life, the possibility of contracting scarlet fever again during her life cannot be ruled out." pregnancy. , scarlet fever - therefore also scarlet fever in pregnancy - is transmitted by air. The contagion, therefore, can occur directly through droplets of saliva or other secretions (for example, nasal secretions) emitted with sneezing, coughing or simply through dialogue. In this regard, it is good to remember that patients who have contracted the infection can be contagious even in the 24-48 hours preceding the onset of the first symptoms. For this reason, it can be difficult to prevent any contact with sick people.
In addition to direct contagion, it is also possible to encounter indirect contagion through the manipulation of objects used by infected and sick individuals, such as, for example, dishes, glasses, toys, clothing, towels, thermometers, sheets, etc. Indirect contagion is made possible by the strong ability to survive in the external environment of S. pyogenes which can therefore favor the appearance of scarlet fever in pregnancy even if the pregnant woman does not come into direct contact with sick patients.
caused by scarlet fever in pregnancy are quite similar to those that occur when the infection affects children. Before the onset of symptoms, however, there is an incubation phase lasting about 48-72 hours. After this time, scarlet fever in pregnancy can cause the appearance of symptoms, such as:- High fever;
- Headache;
- Sore throat (pharyngitis is the most common symptom of the disease);
- Hypertrophic and painful tonsils;
- Formation of a whitish patina on the tongue (white strawberry tongue) and tonsils;
- Abdominal pain
- Tachycardia.
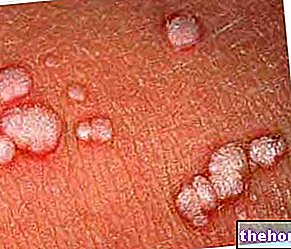
Another characteristic symptom of scarlet fever is represented by the appearance of patches of scarlet red color (scarlet exanthema, hence the name of the disease) in different areas of the body. Fortunately, contrary to what happens in other similar diseases (such as, for example, chickenpox), the aforementioned patches are not itchy and do not cause great discomfort to the patient.
The scarlet rash usually appears within 12-48 hours from the onset of the first symptoms. In this time interval, the whitish patina that covers the tongue begins to change and - as a result of peeling processes - becomes red and wrinkled and, for this reason is defined as "raspberry tongue".
The scarlet rash lasts a few days, after which it disappears giving rise to a furfuraceous desquamation.
The symptomatology induced by scarlet fever in pregnancy - as well as that of scarlet fever that occurs in other adults and in children - is quite characteristic, therefore, easily recognizable. Therefore, should the pregnant woman manifest any of the aforementioned symptoms, it is necessary to contact the doctor or gynecologist immediately.
it is quite a rare event. In this regard, it has been estimated that children born to mothers infected with group A beta-haemolytic streptococcus are infected with the same microorganism in 1% of cases.However, should the bacterium responsible for scarlet fever in pregnancy give rise to vaginal colonization, there is a real risk of undergoing premature rupture of the membranes and preterm birth with all the consequences of the case.
Furthermore, if the beating is also present in the vagina and is not adequately treated, during delivery it could come into contact with the fetus, infecting it. This eventuality, as we have seen, is quite rare but not impossible. For this reason, it is always good to perform a vaginal swab in order to determine the presence of S. pyogenes. This "operation, however, is also useful for identifying the presence of other pathogenic microorganisms, such as the S. agalactiae or group B beta-hemolytic streptococcus (for more information, read: Streptococcus in Pregnancy).
to identify exactly which pathogenic microorganism caused the symptoms.
This diagnostic test is used above all in case of uncertainty and in the presence of unclear symptoms (for example, a slight scarlet rash, absence of typical symptoms such as fever and the presence of the characteristic white patina on the tongue and tonsils, etc. .).