and the manifestation of pityriasis rosea.
In any case, the disease represents 2% of all dermatoses and, in the general population, registers an "incidence equal to 0.14%. The recurrent forms of Gibert's pityriasis rosea are infrequent and, among the pityriasic dermatoses, these they occur in only 3% of affected patients.
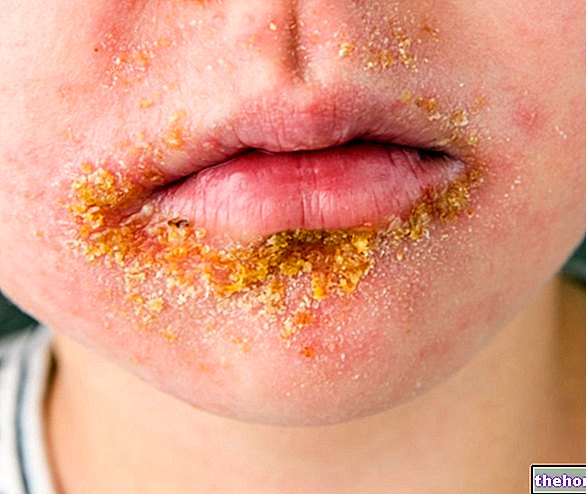
Gibert's pityriasis rosea begins with a typical reddish macula, called mother spot or Gibert's medallion, which represents the sign of recognition of the disease itself.
The mother spot is rounded, with a diameter of 1-3 centimeters; the outlines appear quite defined, although they tend to peel. The fulcrum of the spot appears red-pink (hence the "rosy" name) and, as you move away from the center, the color tends to fade; after a few days from the onset, in general, new satellite spots appear (daughter spots) that spread from the mother spot, whose dimensions are smaller. In rare cases, pityriasis rosea manifests only a "single large red spot.
In only 25% of affected subjects, pityriasis rosea causes itching; in the remaining 75% the disease manifests itself without any appreciable prodrome: the symptomatological picture, in general, is of little entity.

Generally, the daughter spots are arranged symmetrically to the mother spot; very few cases of pityriasis rosea on the legs, genitals and face. , albeit minor, which results in the disappearance of the spinous layer of the epidermis. Furthermore, in some affected subjects, a mild spongiosis is diagnosed (skin alteration characterized by the formation of small blisters or bubbles).
Sometimes, Gibert's pityriasis rosea causes superficial edema, characterized by infiltration of lymphocytes, neutrophils, histiocytes and eosinophils and by dilation of the capillaries [from Treatise on clinical anatomy, By M. Raso].
presumed and demonstrable, but not entirely certain and proven. At the end of the nineteenth century, scholars considered plausible the hypothesis according to which Gibert's pityriasis rosea was connected to syphilis, considered the analogy with the mother spot - already discussed in the previous paragraph. This hypothesis was soon abandoned, as well as the close correlation between fleas and pityriasis rosea, formulated by other researchers of the time [taken from www.ildermatologorisponde.it]
In the nineties of the twentieth century, another possible causal hypothesis was formulated, however soon refuted: it was believed that Gibert's pityriasis rosea was due to a "bacterial or parasitic infection.
Nowadays, the most probable etiopathological assumption of pityriasis rosea, at the same time less questionable, is attributed to two strains of Herpes virus (HHV6 and HHV7), responsible for the sixth disease, a typical critical rash of childhood (skin rash characterized by vesicles, bubbles and pustules).
Probably, frequent contact with particular substances (eg chemical agents, powders, etc.) could stir up dermatosis, also generating cutaneous xerosis; however, these potentially irritating agents are unable to unleash pityriasis rosea without the Herpes virus.
Considering that the triggering factor of pityriasis is a virus, at first glance one might think that the disease is contagious; in reality, Gibert's pityriasis rosea turns out to be only ideally infectious since, in reality, the contagiousness is minimal or even zero.
Other articles on "Gibert's Pityriasis Rosea"
- Gibert's Pityriasis Rosea: Diagnosis and Therapies
- Gibert's drugs for the treatment of Pityriasis Rosea
- Gibert's Pityriasis Rosea in Brief: Summary of Gibert's Pityriasis Rosea