Edited by Doctor Alessio Dini
In 2011, first in Germany and then in France, there was a large number of foodborne infections due to Escherichia Coli. In Germany, the bacterium caused 38 deaths and infected over 3,000 people; in France, 7 children aged between 20 months and eight years were hospitalized with severe intestinal symptoms after eating hamburgers.

In this context, food infections, toxic infections and intoxications are recognized.
MTAs mainly manifest themselves with a symptomatology called gastroenteritis.
Gastroenteritis is an "inflammation of the digestive system which in acute form typically manifests itself with the sudden onset of diarrhea, mostly associated with high fever (38-39 ° C) and abdominal pain, spread throughout the abdomen, which only some subside with defecation. Vomiting often coexists (especially in the case of food poisoning) and general signs of infection, for example muscle pain, headache, nausea and lack of appetite. Stool may be completely liquid, soft or semi- formed, often mixed with mucus.In particular cases the feces can be mixed with blood, in this case we are talking about dysentery.
The best known food infections are those caused by the bacteria Salmonella, Shigella, Campylobacter, Yersinia enterocolitica, Escherichia coli and by the Rotavirus, Adenovirus and Norwalk viruses.
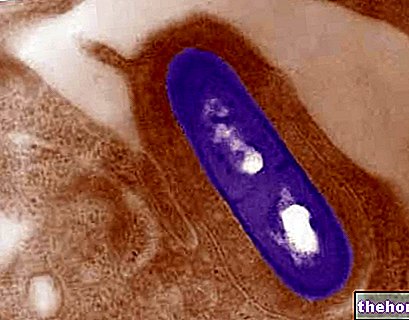
The "killer bacterium" that caused the recent epidemic in Germany and France belongs to the family of enterobacteria (whose natural habitat is the "intestine of" man and / or other animals), genus Escherichia.
Escherichia coli is the best known species of the genus Escherichia. Although over 50,000 serotypes have been typed, most of them are commensal (non-pathogenic) microorganisms while only a small number of strains are capable of inducing disease.
The various serotypes are characterized by different combinations of the antigens O, H, K, F (O: Somatic / parietal; K: capsular; H: Flagellar; F: Fimbriae). It is one of the main species of bacteria that live in the lower intestines of warm-blooded animals (including birds and mammals), contributing to the proper digestion of food. Its presence in groundwater is a common indicator of faecal contamination.
Clinically, there are 5 important groups of Escherichia coli: enteropathogenic, enterotoxigenic, enteroinvasive, enteroadherent and enterohaemorrhagic.
The two recent outbreaks were caused by 2 different strains of this bacterium:
- The German bacterium is called E. coli O104: H4 and before the epidemic in Germany it was already known, although very rare. Belonging to the group of enteroadherent Escherichia coli "EAggEC", this strain expresses adhesion factors capable of promoting colonization of the small intestine, with stimulation of mucus production. This forms a biofilm capable of isolating and aggregating the bacteria. Following the aggregation there is a reduction in the length of the microvilli, mononuclear infiltration and haemorrhage.
The novelty is that this bacterium, following a mutation, has acquired the ability to produce a very dangerous toxin defined shiga toxin, which can cause hemorrhagic colitis and hemolytic uremic syndrome (HUS).
On the other hand, the French strain, belonging to the group of Escherichia coli enterohaemorrhagic "EHEC".
- E. coli O157: H7 (this is its name): it was first identified as a pathogen in the U.S.A. and Canada in 1982, following an epidemic of hemorrhagic diarrhea associated with the consumption of hamburgers in fast food restaurants.
Its peculiarity is its high resistance to low temperatures; in fact it can withstand a temperature of -80 ° C for nine months. Another important characteristic, which can affect the ability to colonize the human intestine, is its resistance to stomach acid. Fortunately, this pathogen is very sensitive to high temperatures (44-45 ° C), so it is essential to properly cook food to make it safe.
Main virulence factors of Escherichia coli O157: H7 are the 2 toxins produced Stx1 and Stx2 which first cause damage to the cells of the intestinal mucosa (enterocytes) and then, entering the circulation, damage above all the kidneys, compromising their functionality.
Therapy, in both adults and children, is based on rehydration and correction of electrolyte alterations, acid-base balance and any blood losses. Antibiotic therapy is not recommended as it can increase toxin release and aggravate the general condition of the patients to whom it has been administered. The most critical patients require intensive treatment based on dialysis, blood transfusions up to kidney transplantation.