Generality
Basal cell carcinoma is a malignant skin tumor, different from melanoma. As the name suggests, this neoplasm originates in the basal cells, which reside in the outermost layer of the skin, or the epidermis.

Figure: Skin lesion associated with basal cell carcinoma. From the site: www.myvmc.com
As with any tumor, one or more genetic mutations cause basal cell carcinoma; these are often the result of excessive exposure to the sun's UV rays, but not only that. The risk factors, in fact, are different.
Basal cell carcinoma manifests itself with a mark on the skin visible to the naked eye and with particular characteristics.
With early diagnosis and prompt treatment, recovery is possible. Conversely, if the diagnosis and treatment are late, it is possible for metastases to form and the basal cell carcinoma to become fatal.
What is basal cell carcinoma?
Basal cell carcinoma, also known as basal cell epithelioma or basalioma, is a malignant skin tumor that originates in the basal cells of the epidermis.
Belonging to the category of so-called skin cancers other than melanoma, it is not a particularly aggressive and dangerous carcinoma, but it can become one when it is not diagnosed and treated in time.
What are basal cells? What tasks do they perform?
The basal cells are cubic or cylindrical cellular elements, located at the base of the epidermis, in direct contact with the underlying dermis. The epidermis is the outermost layer of the skin and is composed not only of the basal cells, but also of other cells.
The basal cells are considered a sort of stem cells, as, by replicating in a very intense way, they are capable of giving life to the so-called keratinocytes, that is the most representative cellular elements of the epidermis. As soon as formed, the keratinocytes move from the base towards the epidermal surface, replacing those of the old generation, produced previously.With this fine mechanism, the basal cells guarantee an effective and periodic cell turnover.
WHAT ARE SKIN CANCERS OTHER THAN MELANOMA
Skin cancers other than melanoma (or non-melanoma skin cancers) are the most common skin cancers, and among the most widespread in general. The common element is the involvement of the most superficial layers of the skin; what differentiates them is the type of cell affected by the neoplasm.
The most common skin cancers other than melanoma are two carcinomas: the basal cell carcinoma, which we are talking about, and the squamous cell carcinoma, also known as squamous cell epithelioma.
EPIDEMIOLOGY
Skin cancers other than melanoma. Squamous cell carcinoma and basal cell carcinoma represent, respectively, 20% and 75% of all skin cancers other than melanoma (the remaining 5% is shown in the table).
The remaining 5% of non-melanoma skin cancers consist of:
- Merkel cell carcinoma
- Cutaneous T-cell lymphoma
- Cutaneous B-cell lymphoma
- Sebaceous gland carcinoma
- Kaposi's sarcoma
- Dermatofibrosarcoma protuberans

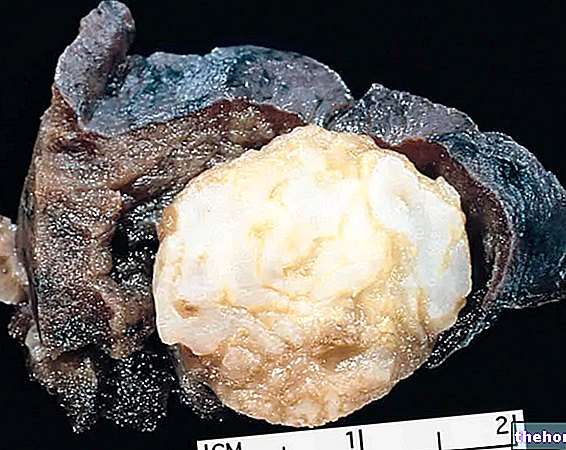
Figure: a basal cell carcinoma compared to a squamous cell. From the site: www.veteranstoday.com
This means that, out of 10 patients with skin cancer other than melanoma, 7/8 suffer from basal cell carcinoma and 2 from squamous carcinoma (the remaining part suffers from the remaining 5%). In Italy, the annual incidence of non-melanoma skin cancers is 100-105 cases per 100,000 inhabitants.
Basal cell carcinoma. Basal cell carcinoma is the most common cancer in the white-skinned population. It usually occurs in middle-advanced age, around the age of 50-60, and affects males more than females.
The incidence rate depends on the geographical area considered: in the areas closest to the equator and / or at high altitudes it is higher than elsewhere. In Italy, the annual incidence is about 75-80 cases per 100,000 people.
N.B: according to some reliable sources, in Europe (therefore also in Italy), the annual incidence of non-melanoma skin cancers is increasing.
Causes
What is a tumor?
A tumor is the result of out-of-control cell multiplication triggered by one or more genetic DNA mutations. In other words, when DNA undergoes certain changes and these changes are irreparable, then the cells that contain it undergo excessive and unstoppable growth and breakdown.
In the case of basal cell carcinoma, the cells that grow and multiply without control, due to one or more genetic DNA mutations, are the basal cells of the epidermis. Thus altered, these cells no longer guarantee that fine mechanism of cell turnover that distinguishes healthy counterparts.
WHAT DETERMINES GENETIC MUTATIONS IN BASAL CELLS?
In most cases, genetic mutations occur due to "excessive exposure to ultraviolet (UV) radiation from the sun and / or tanning lamps.
In rarer cases, genetic damage is due to a depression of the immune system (i.e. a weak immune system) or to direct contact with certain toxic substances.
RISK FACTORS
After years of research, several conditions have been identified that can favor the onset of basal cell carcinoma. These risk factors are:
- Clear skin. Basal cell carcinoma can affect anyone, regardless of skin color. However, those with less melanin (skin pigment that protects the skin from UV rays) are more predisposed than those with more. Hence, light-skinned individuals burn in the sun very easily and, again due to the scarcity of pigment, are also at high risk of basal cell carcinoma.
- Too much sun. Excess exposure to the sun, even if you do not have fair skin, favors the onset of basal cell carcinoma and, in general, all skin cancers.
- Excessive exposure to tanning lamps. Tanning lamps give off the same ultraviolet radiation as the sun. Therefore, exceeding in their use favors the possibility of getting sick with basalioma and, in general, with any skin tumor.
- Radiation therapy (i.e. based on radiation). Some therapeutic methods use ultraviolet radiation to treat dermatological diseases. An excessive dose of these radiations, for example due to prolonged treatment, favors the appearance of skin tumors.
- Personal history of a previous skin cancer. Anyone who has already suffered from basal cell carcinoma or any other skin cancer is a person at increased risk.
- Family history of basal cell carcinoma. Those who come from a family in which one or more members have been affected by a basal cell carcinoma, is predisposed to get sick with the same disease.
- Contact with arsenic. Arsenic is a toxic chemical element that can be found in the air, groundwater and soil. Those who come into contact with high doses of arsenic are predisposed to get sick with various cancers, including basal cell carcinoma.
- Weak immune system. The immune system of an individual is its defensive barrier against infections and other threats, brought from the external environment; in people where it is weak (immunosuppression), it favors the appearance of various disorders, including skin cancers. An emblematic case, of what has just been said, is represented by leukemia or lymphoma patients and organ transplant recipients, who - being forced to suppress their immune system with special drugs - expose themselves to infectious diseases and, in fact , skin cancers.
- Genetic predisposition. Some genetic diseases favor the onset of basal cell carcinoma; in particular, it is the Gorlin-Goltz syndrome and the xeroderma pigmentosum.
Those who suffer from xeroderma pigmentosum are extremely sensitive to sunlight, so much so that they must protect themselves from the sun's rays even inside their own home. - Old age. The most affected are individuals aged 50-60.
Symptoms and Complications
For further information: Symptoms Basal cell carcinoma (or basalioma)
Basal cell carcinoma is characterized by a particular cutaneous sign.
This sign usually appears in the parts of the body most exposed to the sun (such as the face, back of the hands, scalp, neck and ears); however it can appear anywhere, so even in unexpected areas, such as the inside of the mouth, genitals, anus and toes.
Initially the lesion is very small, then, over time, it can also take on considerable dimensions and extend in depth.
WHAT DOES THE SKIN SIGN LOOK LIKE?
The cutaneous sign can present itself with various characteristics. In fact, it can look like:
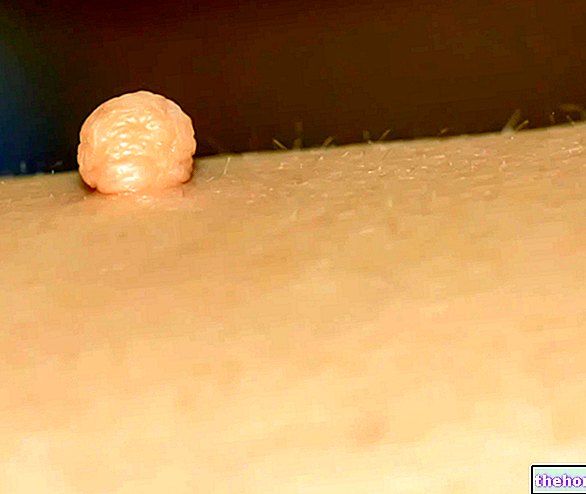
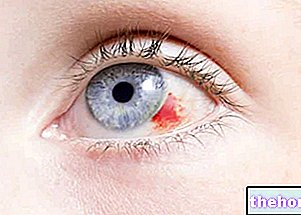
- A pearl white or waxy white bump, in which the blood vessels that pass through it can be easily recognized. Basal cell carcinomas that arise on the face, neck and ears have such appearance. In some cases, the bump tends to bleed and form a crust.
- A "scaly area, not particularly prominent, brown or flesh colored. Basal cell carcinomas that appear on the chest and back have these characteristics. In the long run, the lesion could enlarge considerably."
- A waxy white scar. This aspect, which makes basal cell carcinoma difficult to recognize, is that typical of a very invasive tumor form, called morpheiform or sclerosing basal cell carcinoma.

Figure: a basal cell carcinoma in which the blood vessels passing through it can be recognized. From the site: www.ohniww.org
WHEN TO SEEK YOUR DOCTOR
A dermatological examination is recommended if a skin sign, which appeared for no obvious reason, always tends to show the same characteristics or even worsen.
COMPLICATIONS
Basal cell carcinoma can become an aggressive and lethal malignancy if it is not diagnosed and treated in time. In fact, in such circumstances, it is easier to observe a spread of cancer cells (metastasization), which first contaminate the neighboring tissues, then the lymph nodes and, finally, the other internal organs (such as the liver).
N.B: metastasis is the serious process that gives rise to metastases.
Metastases are cancer cells that have moved from their original location and moved elsewhere, contaminating other organs and tissues in the body.
Special case. Individuals with weak immune systems and those suffering from xeroderma pigmentosum or Gorlin-Goltz syndrome deserve a separate discussion. These subjects, being particularly predisposed to developing a large number of skin cancers, are more difficult to cure, therefore the risk of tumor metastasization is higher.
Diagnosis
Diagnosing basal cell carcinoma early guarantees a greater chance of recovery, as it allows you to start therapeutic treatment earlier. This is why, when in doubt that a particular skin sign may be a tumor, it is advisable not to hesitate to contact your doctor.
The diagnosis process is very simple and quick; in fact, it generally involves a physical examination and a biopsy.
OBJECTIVE EXAMINATION
During the physical examination, the dermatologist examines the suspicious skin area and also analyzes the rest of the body; moreover, by asking the patient about his medical history, he tries to understand whether or not he is a subject at risk of skin cancer.
BIOPSY
The physical examination provides various useful information, sometimes unambiguous, but the only way to establish with certainty the true nature of the skin sign, also identifying the type of cells affected by the tumor, is the biopsy.
It involves the removal, directly from the suspected skin area, of a small portion of tissue and its subsequent observation under the microscope. At the instrument, any tumor cells present show easily recognizable characteristics.
Treatment
In order to recover from a basal cell carcinoma, it is necessary to undergo an operation to remove the skin mark formed.
The techniques for removal are numerous and the choice of one rather than another depends on the location, size and severity of the tumor.
Here is a description of the most used therapeutic approaches in case of basal cell carcinoma:
-
Figure: instrument for electrodissication. Curettage and electrodissication.It is a surgical intervention, which involves curettage (or curettage) of the superficial part of the tumor, followed by burning (electrodissecation) of the base of the carcinoma. The scraping and burning are carried out, respectively, with a tool called "curette"and with an electric needle.
Not recommended for skin neoplasms formed on the face, curettage and electrodissecation represent an ideal therapeutic solution for very small basal cell carcinomas (less than a centimeter) and located on the legs. - Surgical excision (or excision). It is the surgical removal of the tumor area, performed by surgical incision. It is a moderately invasive operation, as the surgeon, to be sure of totally eliminating the basal cell carcinoma, must also cut a part of the surrounding healthy tissue. there is a real possibility that a scar will form.
- Mohs surgery. It is the elimination of the neoplastic sore layer by layer. By examining, from time to time under the microscope, each removed layer, the surgeon knows when the basal cell carcinoma has been completely eliminated. This procedure, since it ends with the observation of the first layer free of tumor cells, it guarantees the exclusive removal of the tumor, without excessively compromising healthy tissues.
- Cryotherapy. It is cold therapy ("crio" comes from the Greek and means "cold"). It involves the use of liquid nitrogen, which, once applied to the basal cell carcinoma, freezes and kills the tumor cells. Cryotherapy is suitable for very thin and not deep neoplasms.
- Topical treatment. It consists in applying, on the affected area, creams or lotions containing particular anticancer drugs, known as imiquimod and fluorouracil. The topical treatment is suitable in case of superficial and small basal cell carcinomas.
- Photodynamic therapy. It involves the use of a photosensitizing drug, for topical use, and a source of light radiation. The photosensitizing drug is a kind of cream which, applied to the tumor area, makes the latter more susceptible to light; the light source, instead, it emits the light necessary to destroy cancer cells, which have become photosensitive after applying the drug. The main advantage of this method is the low invasiveness; the disadvantage is that its long-term effects are unknown (given the deleterious effects of light on healthy cells).
- Radiotherapy. By projecting a very high energy X-ray beam on the tumor area, the tumor cells are permanently damaged, which are thus destined to die. It does not always provide the desired results and, if the treatment is not successful, it is necessary change the method of treatment, the long-term effects are not known.
Prognosis and prevention
Basal cell carcinoma is a tumor that can be cured and from which it can be cured, especially if it does not arise in delicate locations and / or in depth and if it is diagnosed early and treated appropriately.
This, however, does not exclude the possibility that a second skin cancer (the same or of another type) may appear; in fact, an individual who has already been affected once is probably a subject predisposed to this type of neoplasms.
PREVENTION
Basal cell carcinoma is a cancer that can be prevented by following certain recommendations. Here are the main ones:
- Avoid exposing yourself to too much sun in the central hours of the hottest days. In these moments, in fact, the UV radiation is considerable and highly harmful to the skin.
- Use protective sun creams. Their use is particularly encouraged to light-skinned individuals who are at the seaside, to those who carry out an "outdoor work" activity and to people at high risk of skin cancer (people with a weakened immune system, patients with xeroderma pigmentosum). etc).
- Cover the parts of the body that are usually most exposed to sunlight and wear sunglasses. For both of these tips, the same goes for sun protection creams: they must be followed by everyone, but especially by certain people who are most at risk.
- Do not abuse tanning lamps or, better still, avoid using them. Its use is strongly discouraged, especially for those who have fair skin or who are predisposed to skin cancer.
- Check your skin periodically. It is good to examine, from time to time, the whole body, even the most unthinkable points (genitals, between the toes, etc.). It may be useful to have more mirrors, in order to inspect even the most hidden or invisible parts of the body.
- Do not overlook any skin abnormalities that appear suddenly, as it could be basal cell carcinoma or any other skin cancer.






.jpg)