" first part
The thin alveolar walls are devoid of muscle tissue; consequently, the lung cannot contract, but is obliged to passively follow the changes in the volume of the rib cage. The presence of numerous elastic fibers in the connective tissue interposed between one cell and the other guarantees a certain degree of elasticity and resistance to movement.
While the alveoli are responsible for the exchange of respiratory gases, the bronchi and upper airways (nose, pharynx, larynx and trachea) perform various functions, which go far beyond simple transport. These activities have the purpose of protecting the whole organism from foreign materials and the alveoli from too cold or dry air flows; the filtering and conditioning activity is more effective if breathing takes place through the nose rather than the mouth ..
On a macroscopic level, the lungs appear covered with a special lining called the pleura. It is a serous membrane consisting of two sheets; the parietal one internally covers the thoracic cavity and the upper face of the diaphragm, while the innermost (visceral) one adheres to the external lung wall.

The presence of the pleural fluid, a bit like a thin film of water interposed between two glass plates, allows the two pleural sheets to slide and keeps them united and "glued" together. Thanks to this bond, the lungs remain slightly stretched even during exhalation and cannot collapse on themselves. Finally, and most importantly, the adhesion of the pleura to the rib cage and diaphragm allows the transfer of respiratory movements to the lungs.
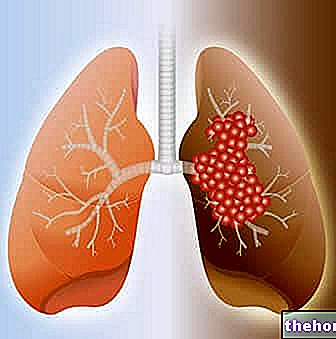
When the pleura becomes inflamed (pleurisy) the contact surfaces of the two sheets lose their characteristic smoothness and the respiratory act gives rise to a painful but also noisy friction (auscultated by applying the ear against the rib cage).
If for some reason (traumatic, spontaneous or therapeutic) air enters the pleural cavity, the adhesion between the lung and the internal thoracic walls is lost; due to the presence of elastic tissue, the lung retracts, significantly reducing its volume and causing dyspnea; this condition is called pneumothorax.
The volume of the lungs varies from individual to individual, in relation to age, sex and body size. In the adult it reaches values between 3.5 and 7 liters; however, during a normal breath, only 500 ml of air are exchanged, which can reach 2.5 - 5.5 liters (vital capacity) maximizing the inhalation and exhalation phases.
At the end of a "maximal exhalation, a certain volume of air remains inside the lungs and airways, which can be estimated at 1000 - 1200 ml (the so-called residual volume). The monitoring of these ventilatory parameters is of enormous importance." in clinical and sports fields (see spirometry).
In addition to an increase in the volume of inhaled and exhaled air, during the physical exercise there is an acceleration of the respiratory acts, which pass from the canonical 12-20 per minute up to 60 or more. The ability to increase the ventilatory frequency is greater in trained than in sedentary and, even more so, in the obese, while the vital capacity is influenced above all by genetic and constitutional factors.

.jpg)