Foot mycosis can be found all year round, not just in summer. Common habits and daily activities that we carry out throughout the year could increase the risk: walking barefoot in the pool, sauna, Turkish bath or beach, as well as the attendance of public changing rooms and showers in gyms and campsites.
Even the use of occlusive and not very breathable stockings and shoes can facilitate the establishment, thanks to sweating, of mycosis in the feet.
and molds and, in most cases, involve one or more nails and / or the most superficial layers of the skin.
Fungi (or fungi) are a group of microorganisms widespread in the environment, already present on human skin. As a rule, these do not constitute any problem, since they almost always coexist in the state of saprophytes, without causing damage; at the same time, the skin surface and the immune system exercise their natural "control" and defense capabilities. In some conditions favoring their abnormal proliferation, however, fungi can turn into invasive pathogens and behave like opportunistic microorganisms, capable of "exploiting" a weakened state of the organism. Other fungi, on the other hand, come from the external environment, breaking the balance and giving rise to mycosis.
The epidemiology varies from one form of mycosis to another and is largely influenced by multiple environmental and individual factors, including: poor hygiene, hot-humid environments, excess and stagnation of sweat, changes in skin pH, local "trauma", circulatory problems and "immunosuppression". In particular, mycoses on the feet are more likely to be found during the summer, since the high humidity and the warm temperatures typical of the season predispose their growth and easier spread among individuals, also considering the frequentation of crowded places. such as swimming pools, changing rooms and beaches. It is enough to walk barefoot or come into contact with the scales of skin that detach from the infected areas and disperse in the environment in order to contract a mycosis.
(stratum corneum of the epidermis) and appendages (nails, hairs) where the keratin (protein rich in sulfur) they feed on is abundant. This category includes the species Epidermophyton, Microsporum And Trichophyton. Some dermatophytes have a particular predisposition to infect the feet (tinea pedis) and nails (tinea unguium).
- Yeasts: single-celled and non-filamentous microorganisms that reproduce very quickly, localizing in warm-humid areas of the body, including interdigital spaces and skin folds. The most important yeasts in dermatology are: Candida albicans, Malassezia furfur And Cryptococcus neoformans. Depending on the fungal agent responsible and the affected area of the body, visible skin manifestations may include edema, redness and pinkish-white desquamative patches; itching is almost always present.
- Molds: multicellular and filamentous fungi; the most common pathogenic molds are: Aspergillus, Acremonium And Fusarium. These types of fungi are mainly responsible for deep and systemic mycoses, while, only in rare cases, they cause skin and superficial infections.
, TINEA PEDIS, also known as athlete's foot since it was once more common among those who habitually wore sneakers. Today, many are susceptible to it: in particular, people who wear socks or shoes made with non-breathable materials. The heat and humidity of the area facilitate the proliferation of causal dermatophytes (Trichophyton spp.), which, in particular conditions of heat and humidity, proliferate and attack the keratin, that is the protein that constitutes the horny layer of the skin and nails.
Even the habit of not drying the feet well or washing them too frequently can predispose to tinea pedis; these incorrect habits alter the pH of the skin, which naturally protects against external aggressions. Public showers, swimming pools and changing rooms they are places that can favor, especially in summer, the spread of mycosis to other people.
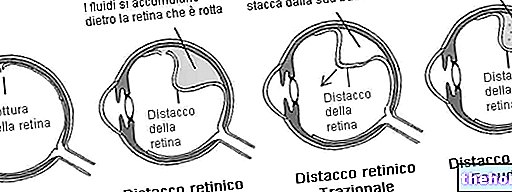
These same risk factors can be at the origin of ONYCHOMYCOSIS, a nail infection caused by dermatophyte fungi and, in a minority of cases, by molds and yeasts. These microscopic pathogens are capable of penetrating, settling and proliferating in tissues rich in keratin, in the space between the lamina and the nail bed. As a result, the nail affected by onychomycosis becomes dull, thickened and prone to flaking or breaking.
Onychomycosis occurs more easily on the toenails than on the hands, since they are more exposed to the conditions that favor their onset. Inside the shoes, thanks to sweating and the use of poorly breathable socks, the ideal habitat for the proliferation of fungi is formed.
To underline is the significant comorbidity between these two mycoses: a third of people affected by onychomycosis of the toenails also suffer from athlete's foot.
and of the site involved (sole of the foot, interdigital spaces, nails, etc.), while the virulence of the fungus and the predisposition of the host determine its severity.- Tinea pedis mainly affects the spaces between the toes and / or the soles of the feet. This dermatophytosis initially manifests itself with skin maceration, erythema, itching and bad odor. Later, cracking, burning sensation and cracks appear between the toes. Athlete's foot also causes plantar thickening and desquamation. In severe cases, tinea pedis manifests itself with vesicles, ulcers, fissures and erosion of the interdigital and subdigital skin of the feet. These lesions favor the entry of bacteria into the subcutaneous tissue. responsible for secondary infections. If left untreated, the Trichophyton spp. it can also cause concomitant onychomycosis, becoming more difficult to treat; spreading into socks and shoes it can infect other toenails as a result.
- In "onychomycosis," the infected nail becomes dull, thickened and prone to flaking or breaking. Over time, this annoying blemish can turn into permanent damage to the nail, as well as causing pain and negatively impacting the quality of life. Onychomycosis is, in fact, a progressive disease: if it is not treated, infection it can spread to other nails and healthy parts of the skin and, when the fungus is able to penetrate the nail surface, it is more difficult to eliminate. At first, you can only notice small whitish areas on the nail that compromise its aesthetic appearance. However, if not properly managed, the infection increases the nail fragility and deforms the lamina, until it detaches. Onychomycosis can also spread from one nail to the other of the feet or hands and, like other infections fungal, to be transmitted from one person to another.
In general, therefore, to limit the damage, it is good to pay attention to the signs indicative of a foot fungus to treat the infection in an adequate and timely manner.
capable of inhibiting the growth of the skin and nail fungi involved. These specific medicines for the treatment of mycosis of the feet may provide for a topical use (ie to be applied locally, on the part affected by the infection) or for oral administration. For example, minor onychomycosis can be effectively treated with a topical antifungal, in the form of a medicated nail polish, until the healthy nail is regenerated.Oral antifungals are mainly used in skin and nail fungus of greater severity or which do not respond only to topicals and in patients who are uncooperative or unable to adhere to topical regimens for a certain time; the doses and the duration differ according to the sites involved by the infection.
It should be emphasized that foot mycosis does not show a tendency to spontaneous healing and is particularly difficult to eradicate, so implementing antifungal therapy from the early stages of the infection is the best approach to solving the problem.













.jpg)