Generality
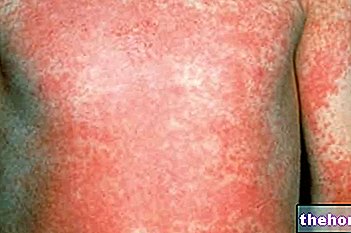
The term "jaundice gravidarum" includes all those gestational situations characterized by an abnormal increase in blood bilirubin, whereby the skin and ocular sclera take on a typically yellowish color.
Causes
The numerous causes that can cause gravidic jaundice are first of all divided into:
- liver disease in pregnancy: causes already present at the moment of conception, which occur during gestation due to external factors independent of it;
- hepatopathies of pregnancy: caused or aggravated by the same gestation.
Intrahepatic cholestasis
Among the liver diseases caused by gestation, the most common cause of jaundice is intrahepatic cholestasis of pregnancy.

Incidence
Intrahepatic cholestasis of pregnancy complicates from 0.8% to 1.5% of pregnancies, manifesting clinically in the second half of gestation; the characteristic symptom is intense itching, associated with jaundice in about 20% of cases. More common in some populations (Chile and Scandinavia), intrahepatic cholestasis of pregnancy has a benign course (it may slightly increase the risk of biliary lithiasis) and disappears after delivery; however, it tends to recur in subsequent pregnancies or with oral contraceptives. Furthermore, it exposes the fetus to an increased risk of premature birth and developmental abnormalities.
The treatment of intrahepatic cholestasis of pregnancy is based on the use of ion exchange resins, such as cholestyramine, which inhibit intestinal reabsorption of bile salts.
Pre-eclampsia
Pre-eclampsia is another "liver disease of pregnancy potentially responsible for jaundice."
It occurs during the second half of gestation, characterized by the significant increase in blood pressure and water retention (the appearance of edema and swelling), for renal damage with possible proteinuria and foamy urine, and for the presence of anemia with reduction of platelets circulating. Pre-eclampsia, a very dangerous condition for both the mother and the fetus, is also characterized by a "hyperbilirubinemia sometimes accompanied by jaundice.
The pivotal symptoms are represented by headache, visual disturbances (for example scotomas) and abdominal discomfort, while in the rarest and most severe cases genuine epileptic attacks occur followed by loss of consciousness. The treatment of pre-eclampsia involves the use of hypotensive and anticonvulsant drugs, up to the artificial induction of childbirth as soon as the fetus is considered sufficiently mature.
Acute fatty liver disease of pregnancy
Acute fatty liver disease of pregnancy is another very serious complication, fortunately rare (1 case every 13,000 pregnancies). Often associated with pre-eclampsia and more common in twin pregnancies, it appears in the last months of pregnancy with symptoms characterized by nausea and vomiting, abdominal pain, general malaise with flu-like symptoms and loss of appetite. Jaundice appears on average one or two weeks after symptomatic onset and can lead to liver failure; also in this case the most effective therapeutic intervention consists in the rapid completion of the birth.
Other Causes of Jaundice in Pregnancy
Among the liver diseases not directly caused by pregnancy we remember the viral hepatitis, quite frequent in developing countries, but fortunately rare in Italy and in industrialized countries.
In this regard, see the articles relating to: hepatitis A, hepatitis B, hepatitis C, hepatitis D and hepatitis E. Other causes are represented by autoimmune hepatitis, chronic liver diseases such as liver cirrhosis and hemolytic diseases (relatively common is HEELP syndrome, a form of anemia characterized by haemolysis, decreased platelets and increased liver function indices, often associated with pre-eclampsia).
A "liver disease typically aggravated by pregnancy is" jaundice from biliary lithiasis, due to the formation of small pebbles (stones) inside the biliary tract. In addition to an "innate predisposition, this phenomenon seems to be favored by the hormonal changes associated with pregnancy. For example, the increase in progesterone reduces the motility of the gallbladder and in general of the entire gastrointestinal tract, while the increase in estrogen is associated with hypercholesterolemia. The most common therapeutic intervention is the laparoscopic removal of the gallbladder.
Symptoms
Whatever the cause, skin jaundice is more evident in light-skinned and anemic patients. It is less evident in patients with dark or edematous skin, for whom higher levels of bilirubin are required in order to be clinically evident.
Since this is a relatively late symptom of liver disease, it is good to report to the doctor any symptoms that suggest the presence of liver disease (loss of appetite; tiredness, malaise and significant weight loss; dark urine or light stools; nausea , vomiting, diarrhea, hypoglycemia, low-grade fever and muscle aches). The appearance of abdominal pain or contractions, localized in the liver (right upper abdominal region) or spread to other abdominal sites, deserves an immediate medical consultation.
Finally, regardless of the presence or absence of jaundice and liver disease, we remember the importance of a diet low in fried foods, animal fats, coffee, tea and of course alcohol (absolutely forbidden in pregnancy), which is useful for lightening the work of the liver during pregnancy. "entire period of pregnancy.
Other articles on "Jaundice in Pregnancy"
- Jaundice
- Jaundice in infants
- Jaundice - Medicines for the treatment of Jaundice
- Jaundice - Herbal medicine
- Diet for Jaundice