In the same way as the intestinal flora, the microenvironment that is created, performs an "important defense function against" the attack of the most aggressive germs, limiting infections
The functionality of the skin flora is predetermined by the genetic heritage, but it can also be influenced by diet, lifestyle and hormonal changes.
When the skin flora undergoes significant changes, the barrier function of the skin is vulnerable and the susceptibility to the appearance of certain skin problems, such as atopic dermatitis, acne or psoriasis, increases.
of many people;Under normal conditions, the resident microbial flora is not pathogenic, while, given the enormous quantity of microorganisms it comes into contact with, the skin can temporarily host also pathogenic or potentially pathogenic species.
Fortunately, our skin has numerous defenses that hinder its colonization by pathogens.
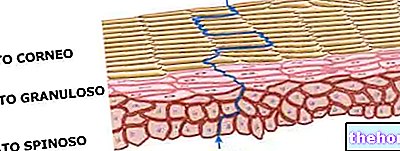
and small imperfections. In reality, this is composed of three main layers, each of which performs different functions and, in turn, are divided into further zones:
- Epidermis (most superficial layer): it is the epithelial layer of the skin, which represents the "external scaffolding of this" organ. Here are the germinative cells, responsible for the production of all skin components.
- In the epidermis, the stratum corneum constitutes about three quarters of the epidermis; it is made up of 20 to 30 cellular lamellae, which resemble overlapping "tiles" ("horny scales") which determine the keratinization of the skin and its protection. The cells that form these laminae have no nucleus and have a hard consistency; each of these elements is destined to detach and fall through desquamation, to be replaced by new cells.
- Dermis (middle part): it is made up of connective, soft and elastic tissue. The dermis is crossed by capillaries, lymphatic vessels and nerve receptors (papillary layer). Furthermore, this portion allows the skin to remain elastic and taut, allowing adequate protection of the whole body (reticular layer);
- Hypodermis or subcutis (innermost layer): connects the dermis and epidermis to the internal tissues, allowing anchoring on muscles and bones and supporting the adherence of the skin during the movement of the body.
What are the functions of the Cutaneous Flora?
The most superficial layer of the skin, known as the stratum corneum, is made up of a dense network of extremely flattened and closely spaced cells, in such a way as to form a real barricade that opposes the loss of liquids and microbial penetration. It is precisely the reduced humidity that significantly limits the growth of this flora, whose density is significantly lower than in other districts, such as, for example, the oral cavity.
Furthermore, every fourteen days, these cells are promptly renewed and, desquamating, bring with them the microbes that settle in the cracks between the horny scales (the most superficial cells of the stratum corneum are so called).
Skin lipids, together with sodium chloride and immunoglobulins present in sweat, contribute to making the skin an inhospitable environment for the vast majority of microbes.
Similarly to what has been seen for the intestinal and vaginal bacterial flora, the microorganisms that make up the skin flora also establish a mutually beneficial relationship with the organism. the skin pH thanks to the degradation of the sebum they feed on. Others, like it Staphylococcus aureus or the Candida albicans, although potentially pathogenic, they do not form colonies numerically sufficient to cause problems to the organism.
Just as the composition of the intestinal microbial flora is influenced by the current and previous dietary habits of the individual, the skin flora is also sensitive to climatic conditions, the degree of personal hygiene, the composition and quantity of sebum and sweat, as well as numerous others factors that can influence their degree and type.
Skin flora: which sites are most colonized?
The typical sites of colonization are the sebaceous glands, which produce an oily mass called sebum, and the hair follicles associated with them; colonization of the sweat glands is more difficult, due to the antiseptic action of lactic acid, sodium chloride and antibodies present in sweat. Anaerobes populate the deepest portion of hair follicles and sebaceous glands, while staphylococci, along with Pytirosporum sp., settle in their most superficial stretch.
Generally speaking, the wettest and most sebum-rich areas, as well as the areas close to the skin orifices, are richer in microbes.Among these microorganisms, there is a small anaerobic Gram negative bacterium, called Propionibacterium acnes, particularly greedy for sebum. From the hydrolysis of cutaneous lipids operated by it, free fatty acids originate which enter the dermis, irritating it and favoring those inflammatory phenomena that are at the basis of acne.
Flora Cutanea: can it spread to other parts of the body?
But the real danger of the skin flora derives from the possibility that these germs can reach the bloodstream or body areas where they are not normally present. This can occur, for example, due to:
- A wound;
- A surgery performed in an inadequately sanitized environment;
- A temporary drop in the immune system.
In these situations there is a radical change in the environmental conditions of the skin; the presence of humidity and necrotic tissue, for example, favors the proliferation of Gram negative pathogens, hindering the growth of Gram positive saprophytes which are the basis of normal skin flora.
: can they depend on the Cutaneous Flora?The metabolism of skin lipids and sweat secretions leads to the formation of substances, such as ammonia and short-chain fatty acids, responsible for bad body odors.
An alteration of the normal skin bacterial flora or its excessive growth, can therefore be the basis of the unpleasant odor typical of some individuals (it is not always and only a problem of poor personal hygiene). In these cases, there are specific deodorants, called bacteriostatic, capable of limiting, but not inhibiting, the proliferation of the skin bacterial flora (since, as we have seen, this is particularly useful in preventing the settlement of pathogens) .