Bone cells and bone renewal
Despite the characteristic mineralization, the bone is far from being dead tissue. On the contrary, it is the site of "intense cellular activity, so much so that every year about 10% of our bone mass is renewed, through physiological mechanisms of neo-formation and resorption. This means that:
- every 10 years the skeleton is completely renewed.
All this involves structural modifications detectable only microscopically and which do not involve macroscopic changes in its shape (at least in adulthood).
Bone cells are didactically divided into four categories: osteocytes, osteoblasts, osteoclasts and their precursors. It is good to remember, from the beginning, that:
- osteoblasts are responsible for the formation of bone matrix
- osteoclasts are responsible for the breakdown of bone matrix
So let's focus on these two cell types. As for osteoprogenitor cells (also called preosteoblasts), it is enough to know that they give rise to other cell types and that they are found in large quantities in the endosteal and periosteal surfaces of the bone.

Osteoblasts
Osteoblasts are cells that specialize in the production of bone tissue.
They have a globosic or polyhedral shape, monostratified; they tend to juxtapose each other, covering small areas of bone matrix, forming the so-called mineralization front.
Osteoblasts synthesize the various tissue components, both fibrous and amorphous, participating in the formation of the osteoid and in the regulation of its mineralization processes.
The osteoid is given by a support of collagen fibers aligned to form an organic matrix, on which the hydroxypatite crystals and other mineral components are bound. The collagen fibrils are arranged according to preferential lines of force, in such a way as to giving the bone properties of resistance to mechanical stress.
In addition to type I collagen, which is assembled into fibrils in the extracellular spaces and acts as a support for mineralization, osteoblasts produce some proteins, such as osteocalcin and osteonectin, which play a "supportive action in the matrix deposition process. calcified.
Osteoblasts are also believed to play a role in the early stages of the resorption process by processing specific proteases and osteoclast activation factors.
Osteoblasts are cells of mesenchymal origin (the mesenchyme is the embryonic connective tissue that gives rise, for subsequent stages of development, to the adult connective tissue).
Osteoclasts
Osteoclasts are large cells, with a diameter ranging between 20 and 100 microns, with many nuclei, mobile and specialized in the resorption of bone tissue.
Thanks to the numerous microvilli, the osteoclasts attach themselves like suckers to a section of the bone matrix; they are generally accepted in small gaps known as Howship's. Here they secrete proteolytic acids and enzymes, digesting both the supporting collagen and the inorganic matrix and solubilizing the minerals it contains.
The resorption of bone tissue operated by osteoclasts plays an important role in the process of regeneration and remodeling of bone tissue, but not only. These cells are in fact important for regulating serum calcium and phosphorus concentrations.
Osteocytes
The secretion of the osteoblasts occurs according to a very precise orientation: initially it is polarized towards the pre-existing bone surface, but at regular intervals it also turns in the other directions; in this way the osteoblasts move away from each other and remain imprisoned in the matrix being mineralized. Once "walled" it substantially slows down its metabolic activity and becomes an osteocyte.
When the osteoblasts have exhausted their function they enter a state of quiescence *, or they transform into less active cells, called osteocytes, which remain trapped in the calcified bone matrix. Taken together, these will make up about 90% of the bone cell stock **.
It seems that the function of osteocytes is to participate in bone remodeling in response to stimuli of various kinds. Under the stimulus of calcitonin and parathyroid hormone, they also participate in the regulation of blood levels of calcium and phosphorus, controlling both the activity of osteoclasts and that of osteoblasts.
(*) When the process of forming new bone is exhausted, some osteoblasts cease their activity, reduce their organelles and transform into a membrane of flattened cells (bone lining cells).
These cells are arranged to cover the bone surface when this is in a phase of quiescence; they are attributed a role in mediating exchanges between blood vessels and osteocytes.
(**) Osteoprogenitor cells, osteoblasts and osteocytes are consecutive functional phases of the same cell type. Osteoclasts, on the other hand, derive from precursors migrated into the bone tissue from the blood, the so-called preosteoclasts, which in turn differentiate from stem cells of the hematopoietic bone marrow.
Other articles on "Osteoblasts, osteoclasts, osteocytes"
- bone tissue
- bone
- bones of the human body
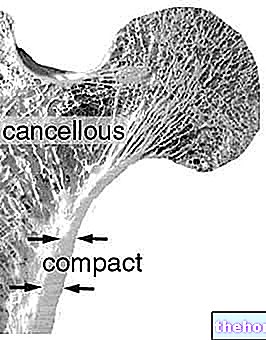
- spongy bone compact bone
- periosteum endosteum
- bone marrow
- bone remodeling
- bone mass
- height growth
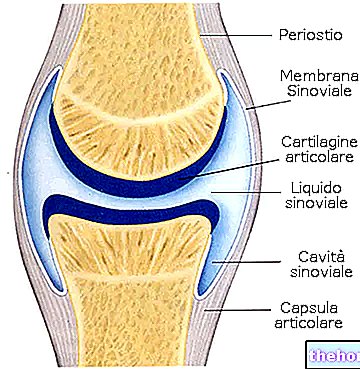
- joints
- Joints: anatomy structure